INTRODUCTION
Thoracolumbar burst fracture is a challenging problem. There are controversies on deciding stability of spinal segment after fracture and also deciding on its management. There is no established guideline for conservative and surgical management. Moreover the indications for operative treatment and type of procedure for stabilization of a thoracolumbar burst fracture remain controversial, especially for neurologically intact patients [2].
The main goal of surgical treatment is to decompress the spinal canal and nerve roots, realign the spine, correct and/or prevent the development of posttraumatic kyphotic deformity, and provide long-term stability of the injured spinal segments [1].
There is controversy on fusing vs. not fusing the spinal segment, short vs. long segment fixation and also on open vs. percutaneous screw fixation. The fixation of burst fractures by posterior approach is generally conducted with posterolateral fusion or posterior fusion. However, other authors [8,10,26,30,33,35,36] reported good results by using open or percutaneous pedicle screw fixation only without fusion.
There are only few literatures available which describes percutaneous screw fixation for thoracolumbar burst fracture [8,26,35,36].
Spinal canal integrity, sagittal balance and anterior column intactness are very important for successful outcome in this type of injury. The treatment modality that provides superior spinal canal restoration has not yet been conclusively identified [16,25].
We treated our patients who had thoracolumbar burst fracture but with intact neurology with postural pillow reduction and lordotic posterior column compressive percutaneous transpedicular screw fixation. This is a low pressure restoration method.
MATERIAL AND METHODS
We retrospectively analyzed 34 patients who had undergone lordotic posterior column compressive percutaneous transpedicular screw fixation for thoracolumbar burst fractures with intact neurology between the time period of July 2008 and June 2012. The inclusion criterion for this study was patients with thoracolumbar burst fracture with intact neurology. The exclusion criteria were (1) patients with thoracolumbar burst fracture but with frank instability in the form of either facet subluxation or dislocation and (2) patients with thoracolumbar burst fracture but with presence of neurological deficit.
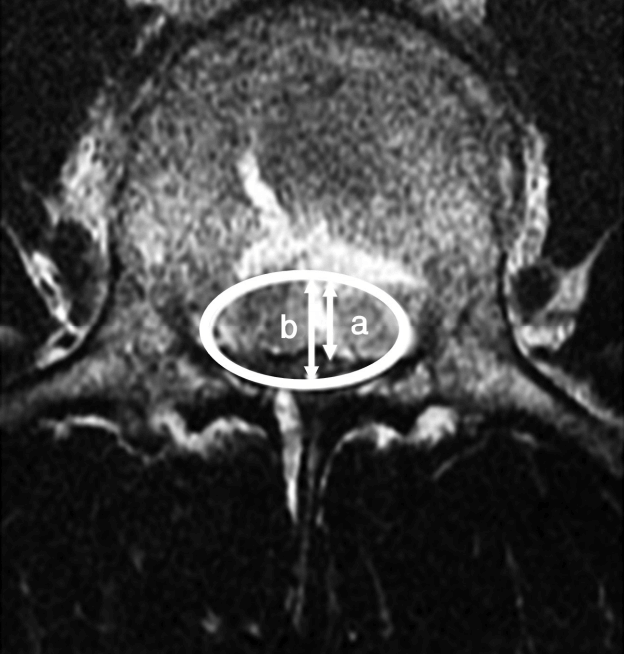
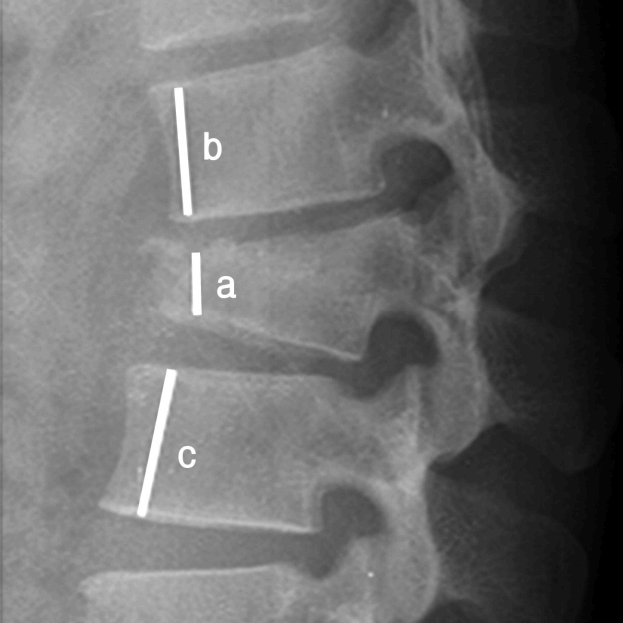
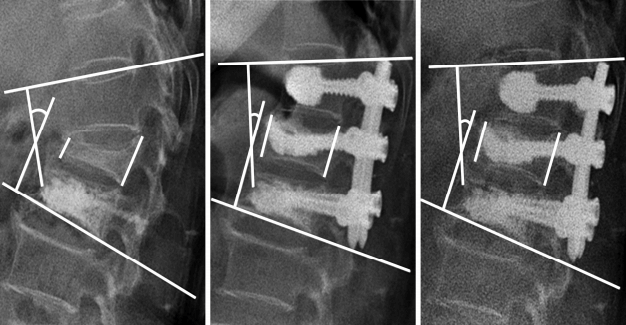
We measured canal size (stenosis), anterior vertebral height, and sagittal (lordotic) angle preoperatively, immediate postoperatively and after 6 months. Canal stenosis was defined in percentage with this formula: Stenosis of canal %=Space occupied by fragment in canal (a)/mid canal diameter (b)X100% (Fig. 1). Reduction in anterior vertebral body height was measured in percentage with this formula: Reduction in vertebral height %= height of fractured vertebrae (a)/0.5Xheight of normal adjacent vertebrae (b+c)X100% (Fig. 2). Sagittal angle was defined as angle formed by intersection of a line passing parallel to superior endplate of cranial vertebra and a line passing parallel to inferior endplate of caudal vertebra (Fig. 3).
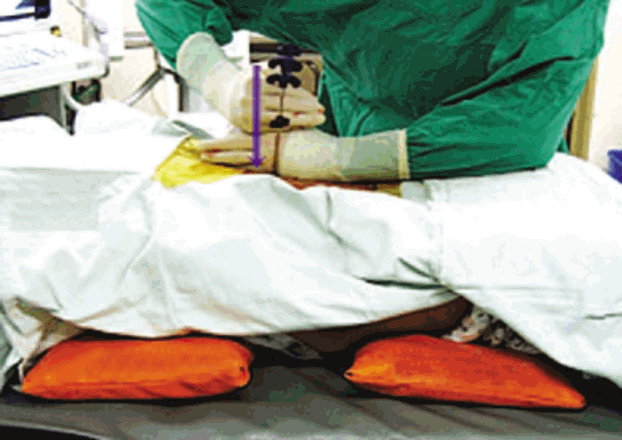
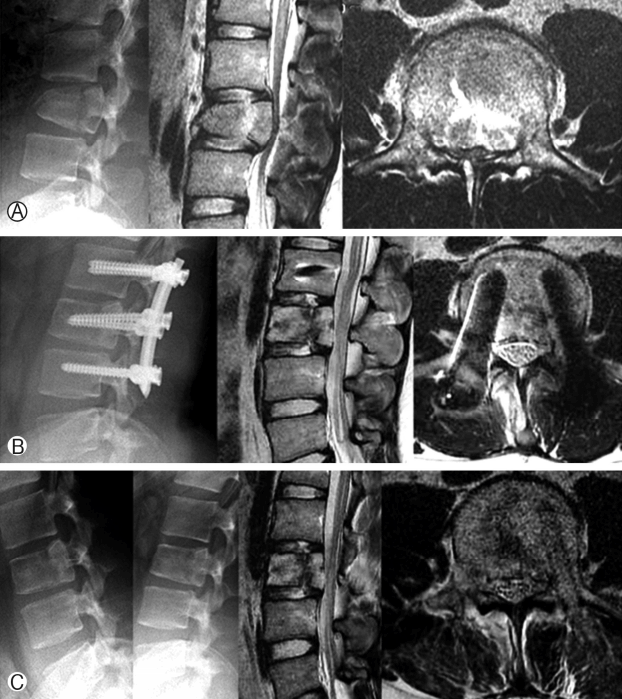
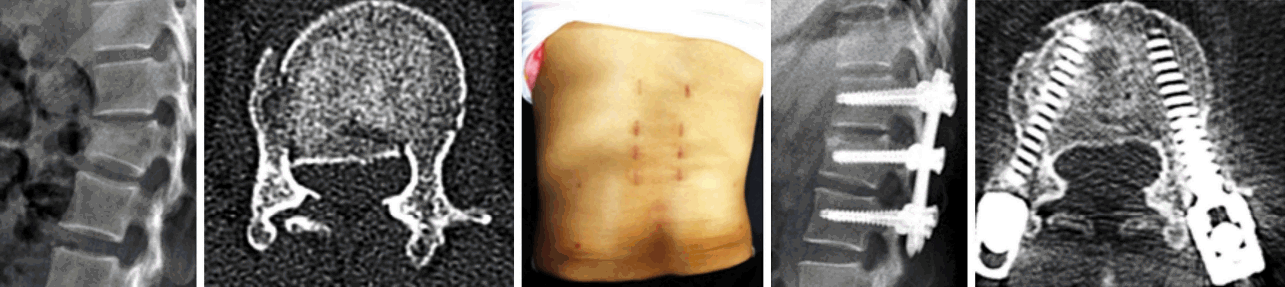
Vertebral height and lordotic angle were measured in X-ray and canal stenosis in magnetic resonance imaging (MRI) or computed tomography (CT).The surgical procedure included three different elements: (1) preoperative postural pillow reduction for 1-2 days (Fig. 4), (2) augmentation of fractured vertebra, and (3) lordotic, posterior column compressive, percutaneous screw fixation (Fig. 5). Preoperatively Pillow was placed at apex of fracture making hyperlordotic condition of spine. Pillow was made by rolling bed sheet. Thickness of the pillow was about 8-10 cm depending upon torso of the patient. Duration of postural pillow reduction (1-2 days) was decided with interval X-ray taken depending upon reduction of burst fragment encroaching spinal canal. The earlier the reduction, the early surgery was done. Patients were made pain free with analgesics. Interval neurological assessment was done. During surgery patient was placed prone on radiolucent table over 2 bolsters. Cranial bolster was placed over chest region and caudal bolster was placed over pelvis region thus allowing abdominal area to be free and also allowing to do anteriorly directed force for further correction of kyphosis while securely fixing connecting rods to pedicle screws. We used the vertical axis percutaneous screw Apollon System (Solco Medical, South Korea) for percutaneous screw fixation. We did short segment fixation with placement of screw in fractured vertebra as well. Pedicle screws were placed in C-arm guidance. Before inserting pedicle screw we had augmented fractured vertebra by polymethylmethacrylate (PMMA) in osteoporotic bone, or non-PMMA materials in non-osteoporotic bone). We had securely fixed rods to screws while applying anteriorly directed force from back to correct sagittal alignment. Ventral decompression was not required in any of our cases with our technique. Implants were removed in 9-12 months in all cases.
RESULTS
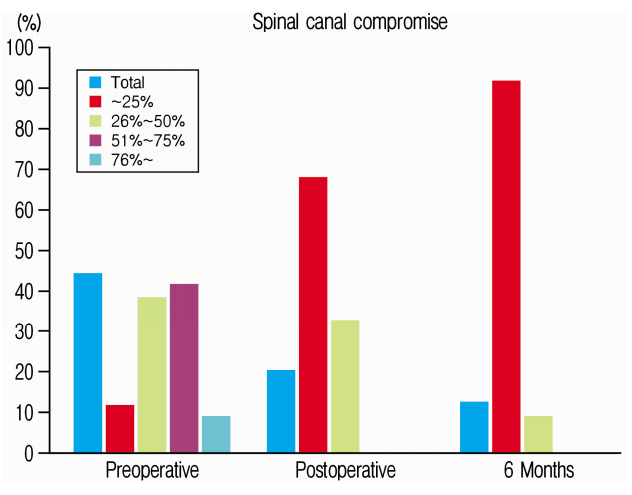
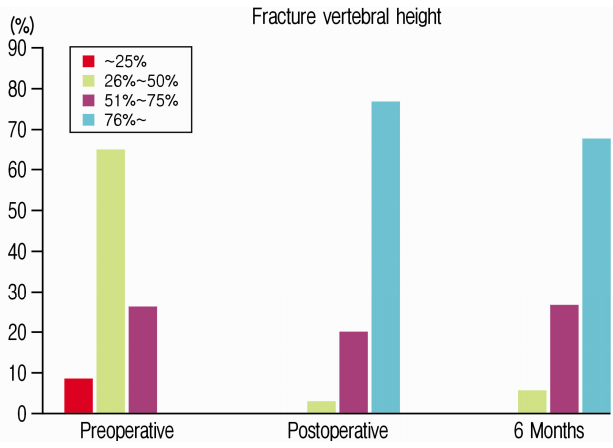
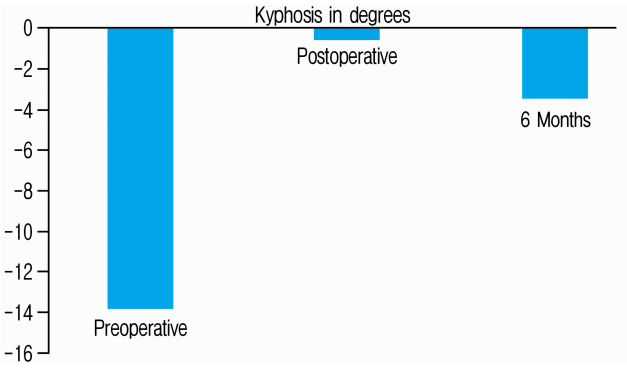
We had total 34 patients, 17 were male. The mean age was 52.03±12.51 years. Most fractured level was L1 (14 patients), followed by L2 (9 patients), T12 (6 patients) and L3 (5 patients). Spinal canal stenosis was 44.37±17.95% preoperatively and were 20.04±9.39% and 12.06±7.46% post-operatively and at 6-month follow-up, respectively. At 6 months, preoperative canal stenosis of 44% remodeled to 12%. Almost 50% of patients had canal stenosis of more than 50% preoperatively. In 91% of patients canal remodeled back to 0 to 25% of stenosis in 6 months (Table 1 and Fig. 6). Likewise anterior vertebral height were 43.91±14.58% (56% reduction), 81.69±13.12% and 77.29±12.83% preoperatively, post-operatively and at 6-month follow-up respectively. At 6 months, preoperative anterior vertebral height of 44% increased to 77%. The anterior vertebral height loss was of 4.4% from immediate postoperative state. 94% of our patients maintained anterior vertebral height more than 50% and 68% maintained more than 75% anterior vertebral height at 6 months follow up (Table 2 and Fig. 7). The spinal lordotic angle were (-13.86)±11.13 degrees, (-0.518)±14.34 degrees and (-3.40)±13.39 degrees preoperatively, post-operatively and at 6-month follow-up respectively. The preoperative average kyphosis of 14 degrees corrected to 0.5 degrees immediate postoperatively but there was loss of lordosis about 2.9 degrees making kyphosis of 3.4 degrees at 6 months follow up. At 6 months 35.29% of patients maintained lordosis at 1 degree and 58.82% maintained sagittal balance between 0-20 degrees. Only about 6% had kyphosis (Table 3 and Fig. 8).
DISCUSSION
Thoracolumbar burst fracture is usually 2 columns and sometimes 3 columns injury and mostly unstable injury and requires stabilization. The indications for operative treatment and type of procedure for stabilization of a thoracolumbar burst fracture remain controversial, especially for neurologically intact patients. Spinal canal integrity, sagittal balance and anterior column intactness are very important for successful outcome in this type of injury. Ideally normal thoracolumbar area has 0 to -10 degrees of sagittal alignment and thoracolumbar junction is essentially 0 degree or slightly lordotic. Radiographic findings of 50% of anterior vertebra body height loss, interspinous process widening and kyphosis of more than 30 to 35゚ were suggestive of posterior ligamentous complex disruption [3,23]. However, less than 50% to 60% anterior vertebra body height loss, absence of neurological deficits and kyphosis less than 30 to 35° were defined as stable injuries [6,20]. Burst fractures should be considered unstable if there is associated posterior longitudinal ligament (PLL) injury in magnetic resonance imaging (MRI) [15,28,29]. AO/Magerl classification is also helpful to define stable and unstable spinal fractures [18].
The main goal of surgical treatment is to decompress the spinal canal and nerve roots, realign the spine, correct and/or prevent the development of posttraumatic kyphotic deformity, and provide long-term stability of the injured spinal segments [1]. Posterior reduction and instrumented fusion without decompression (ligamentotaxis) [3,31], posterolateral decompression and posterior instrumented fusion [24], anterior decompression and instrumented fusion [13,17], and combined anterior and posterior approach [4,9,22] are several methods mostly being practiced for operative management of thoracolumbar burst fractures.
With the invent of minimally invasive spine surgery there are few literature also available on percutaneous fixation of thoracolumbar burst fracture and revealing encouraging results [8,30,33,35,36].
But posterior fixation has some problem like poor initial fixation or secondary loosening in patients with osteoporotic spine.27 Some technical modification such as augmentation of the instrumentation with calcium phosphate bone cement, longer constructs, and use of cementable cannulated screws, screws thread engagement in the pedicle, penetration of the screws through the anterior cortex, and use of larger diameter screws are being practiced to increase the stability of the construct and the screw pullout strength [21,32,37]. Pedcle screws at the level of the fracture site also helps to provide better kyphosis correction. It also saves motion segments and offers improved biomechanical stability [7,14,19]. Study by Canbek U et al. compared intermediatesegment (IS) and long-segment (LS) instrumentation in the treatment for thoracolumbar burst fracture and the measurements of local kyphosis (p=0.955), sagittal index (p=0.128), anterior vertebral height compression (p=0.230) and canal diameter expansion (p=0.839) demonstrated similar improvement at the final follow-up between the two groups. This study also support adequacy of short segment fixation [5].
Taking consideration of all these factors in this study preoperative postural pillow reduction for 1-2 days was done in order to achieve the initial restoration of canal compromise and vertebral height under normal spinal alignment. Fractured vertebral augmentation was done by polymethylmethacrylate (PMMA) in osteoporotic bone, or by non-PMMA materials in non-osteoporotic bone, to maintain the restored vertebral height and to increase the anterior column loading of wolf’s law and lordotic, posterior column compressive percutaneous screw fixation was done using the vertical axis percutaneous screw Apollon System (Solco Medical, South Korea) to achieve the continuous additional restoration of canal compromise under the low loading of wolf’s law to the middle column.
1. Canal Remodeling
With our technique on average 44% preoperative stenosis remodeled to 12% in 6 months. Almost 50% of patients had canal stenosis of more than 50% preoperatively. In 91% of patients canal remodeled back to 0 to 25% of stenosis in 6 months.
In the study conducted by Yang WE et al. [35] using percutaneous pedicle screw fixation canal remodeling occurred from 51±17.2% stenosis to 21±11.6%. Likewise In the study done by Zhang Z et al. [36], the mean vertebral canal diameter increased from 5.5±1.3 to 11.1±2.2 mm (p<0.05) and the mean canal stenosis index increased from 32.9±7.8 to 84.8±7.3% (p<0.05).In other study done by Cimatti M et al. [8] by using lordotizing screw in fractured vertebra, mid sagittal index (MSI) decreased from 44.91% to 11.2% at last follow up (3 years).
Reduction of canal compromise by 50% within the first year after nonoperative treatment, even in patients with neurological injury had been reported by De Klerk [12]. With posterior distraction instrumentation showed a spinal canal clearance ranging from 49% to 72% of normal immediately postoperatively. At final follow-up, the mean canal measurement was 87% of normal [34]. In the study done by Mumford et al. the canal remodeling occurred with the conservative treatment even though nearly 66% of spinal canal was involved [25].
2. Sagittal Balance
With our technique preoperative average kyphosis of 14 degrees corrected to 0.5 degrees immediate postoperatively but there was loss of lordosis about 2.9 degrees making kyphosis of 3.4 degrees at 6 months follow up. At 6 months 35.29% of patients maintained lordosis at 1 degree and 58.82% maintained sagittal balance between 0-20 degrees. Only about 6 % had kyphosis more than 20 degrees.
In the study conducted by Yang WE et al. [35] using percutaneous pedicle screw fixation the kyphosis of 17.1±8.3 corrected to 11±7.4 degrees immediate postoperatively and at 6 months follow up it increased to 13.8±8.6 with loss of 2.8 degrees of lordosis. In the other study done by Zhang Z et al. [36], the local kyphosis angle reduced from 25.9°±3.4° to 6.9°±2.2° (p<0.05) and remained 7.9°±2.0° (p>0.05) with loss of 1 degree lordosis from immediate postoperative status. Likewise in the other study done by Cimatti M et al. [8] by using lordotizing screw in fractured vertebra, kyphotic angle decreased from 5.62 to 0.07 degrees immediate postoperatively but again increased to 0.8 degrees at last follow up (3 years) with loss of 0.73 degree of lordosis.
In all studies including our study there was a loss of lordosis that had been achieved immediate postoperatively.It has been also documented by study done by Mumford J et al. [25] that the posttraumatic kyphosis is progressive regardless of the type of treatment. However,with our technique kyphotic angle correction is better than studies done by Yang WE et al. and Zhang Z et al. But we cannot comment based on study done by Cimatti M et al. as in this study preoperative initial kyphosis was less from the beginning.
3. Anterior Vertebral Height
In our study preoperative average anterior vertebral height was 44% (56% reduction) and it increased to 82% immediate postoperatively. At 6 months follow up it was maintained at 77% with loss about 5% height. 94% of our patients maintained anterior vertebral height more than 50% and 68% maintained more than 75% anterior vertebral height at 6 months follow up.
In the study conducted by Yang WE et al. [35] using percutaneous pedicle screw fixation ,the loss of anterior vertebral height was 42.6±8.3% preoperatively. It was corrected to 22.9±16.5% loss only immediate postoperatively and at last follow up it was maintained at 32.8±18.2% loss with loss about 9.9% from immediate postoperative corrected height.
It seems that with our technique anterior vertebral body height correction is better than study done by Yang WE et al.
Our technique is unique because restoration of spinal parameters is done with staged low pressure gradual restoration taking consideration of all 3 columns. Preoperatively initial restoration is done with postural pillow and in operating room with an anteriorly directed lordotic compressive force. We also augment anterior column with PMMMA or non-PMMA materials to maintain anterior height load bearing characteristics. We also do pedicle screw fixation in fractured vertebra. We recommend this technique in thoracolumbar burst fracture.