Using Swallowing Quality of Life to Compare Oropharyngeal Dysphagia Following Cervical Disc Arthroplasty or Anterior Cervical Discectomy and Fusion
Article information
Abstract
Objective
To evaluate dysphagia outcomes using the swallowing quality of life (SWAL-QOL) questionnaire between patients undergoing cervical disk arthroplasty (CDA) or anterior cervical discectomy and fusion (ACDF).
Methods
Patient-reported outcome measures (PROMs) were collected using SWAL-QOL, VAS, NDI, and SF-12 PCS. All measures were recorded preoperatively to 6-month postoperatively. Patients were grouped according to cervical procedure and instrumentation used. Differences in PROMs and SWAL-QOL domains were evaluated by t-test and one-way ANOVA with post-hoc testing, respectively. Simple linear regression was employed to evaluate the relationship between number of levels operated on and postoperative outcomes.
Results
161 patients were included. CDA patients had significantly worse SWAL-QOL scores at 6-months. Preoperative VAS neck was significantly worse for patients who underwent either an ACDF procedure with a stand-alone cage or CDA as compared to patients who underwent an ACDF with anterior plating. At 6-months postoperatively, CDA patients reported a significantly worse “fatigue” score compared to ACDF patients. At 6-months postoperatively, ACDF patients reported a significantly better “sleep” scores compared to CDA patients with both recipients of an anterior plate and stand-alone cage reporting significantly better scores compared to the CDA cohort (p=0.024; p<0.001). The SWAL-QOL domain of symptom frequency at 6-weeks postoperatively was significantly associated with number of levels operated (p=0.032).
Conclusion
Patients undergoing either an ACDF or CDA procedure largely did not demonstrate differences in pain, disability, and dysphagia scores. However, at more longitudinal timepoints CDA patients reported worse fatigue and sleep scores compared to ACDF patients.
INTRODUCTION
Anterior cervical discectomy and fusion (ACDF) is commonly performed for cervical degenerative spine pathology and is considered an effective form of treatment [1,2]. Cervical disc arthroplasty (CDA) is a comparable procedure to ACDF and its increased use for treatment of cervical spine pathologies can be tied to its reported favorable outcomes [3-5]. However, use of either procedure still places patients at risk for complications such as oropharyngeal dysphagia, tracheoesophageal hematomas, increased radiculopathy, respiratory insufficiency, and esophageal perforation [1], with dysphagia being one of the more common complications [6,7]. In fact, its occurrence rate has been reported to be as high as 8.5% [8], with one study reporting an incidence of 71% within several weeks postoperatively [9]. Although dysphagia is a prevalent postoperative complication, a limited number of studies have explored its effects on a patient’s recovery course [10-12].
Dysphagia often occurs during the more immediate postoperative time period; however, instances of delayed onset are possible and can range from a few weeks, several months, or even as long as 5 years postoperatively [13,14]. Currently, methods for assessing dysphagia are primarily performed clinically and involve the use of videofluoroscopic swallow studies and upper endoscopies [15,16]; Beyond the immediate postoperative timepoint, the psychosocial effects of dysphagia should also be evaluated, which can be accomplished using dysphagia specific patient reported outcomes measures (PROMs). One such PROM used across different patient populations is the swallowing quality of life (SWAL-QOL) questionnaire, which is a validated psychometric with several scales that evaluate the impact of dysphagia on quality of life [17]. The majority of the survey’s scales assess dysphagia-specific quality of life measures, including: burden, eating duration, eating desire, symptom frequency, food selection, communication, fear, mental health, and social. Meanwhile, sleep and fatigue scales of SWAL-QOL assess general quality-of-life. As the questionnaire has demonstrated favorable internal-consistency reliability and short-term reproducibility, with proven sensitivity to clinically defined dysphagia severity, SWAL-QOL is an effective means to evaluate the presence and severity of dysphagia [17]. Other similar PROMs have also been developed, including the HSS Dysphagia-Dysphonia (HSS-DDI) score [18], the M.D. Anderson Dysphagia Inventory (MDADI) [19], the Bazaz Score [20], and the Dysphagia Symptom Questionnaire (DSQ) score [21]. Although useful in their own right, these tools have been reported to have several limitations with being too simplistic [8], not formally validated [22], lacking a preoperative assessment [23], or designed for patients undergoing treatment for malignancy [22].
Yet, even with a number of different dysphagia PROMs to choose from, the literature surrounding the impact of swallowing difficulties on patient quality of life remains underreported within the ACDF and CDA patient population. While a number of investigators have studied the validity of SWAL-QOL within the ACDF population [22,24], others have detailed the ability of dysphagia to severely affect quality of life and act as a risk factor for depression and anxiety [25,26]. As profound as these results are, these studies were conducted primarily on cancer patients and individuals with gastroesophageal reflux disease. Other studies have alluded to the effect swallowing difficulties have on pain and disability and overall quality of life but were either restricted to clinical diagnosis of dysphagia [10], were restricted to deformity patients [11], or utilized a metric other than the SWAL-QOL survey [12]. Therefore, our study aims to address this gap in knowledge by establishing differences in the impact of dysphagia on quality of life between ACDF and CDA patients. Based on substantial previous literature, we hypothesize there will be comparable results regarding incidence of dysphagia but will differ on its impact on patient quality of life.
MATERIALS AND METHODS
1. Inclusion and Exclusion Criteria
In accordance with institutional ethical guidelines, both Institutional Review Board approval (IRB Approval No. ORA #14051301) and written patient informed consent were obtained prior to commencing the study. Eligible participants were identified through a retrospective review of a prospectively maintained surgical database for cervical spine procedures performed between November 2014 and September 2020. Patient inclusion criteria was set as individuals undergoing a primary, elective, single or multilevel ACDF or CDA. Individuals were excluded for undergoing a revision procedure or for a surgery indicated for traumatic, malignant, or infectious etiologies. The purpose of our exclusion criteria was to eliminate potential confounding variables that may significantly bias our final results. Additionally, patients who did not complete a preoperative SWAL-QOL survey were removed from the study. All patients were treated at the same academic tertiary medical institution by a single spine surgeon.
2. Patient Health Information
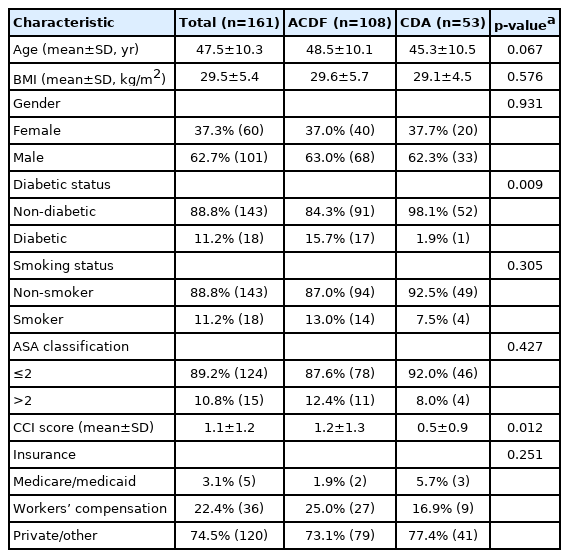
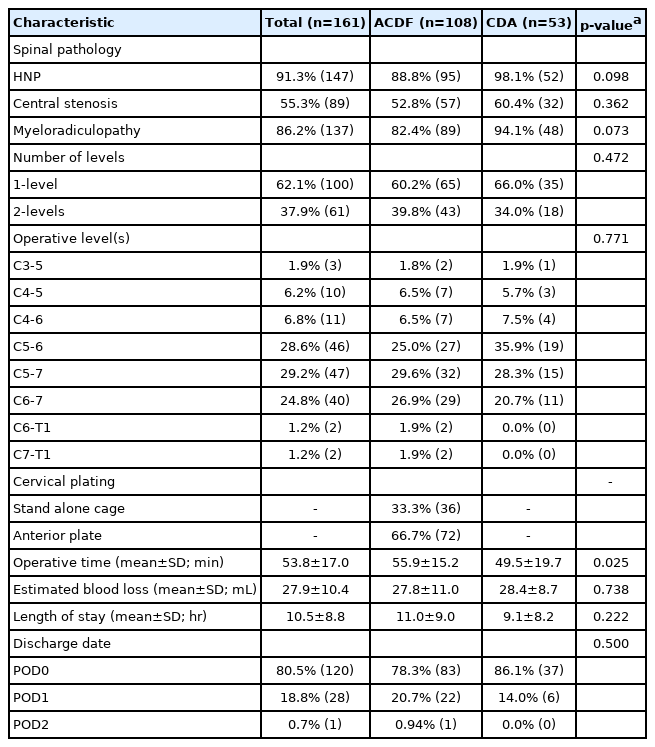
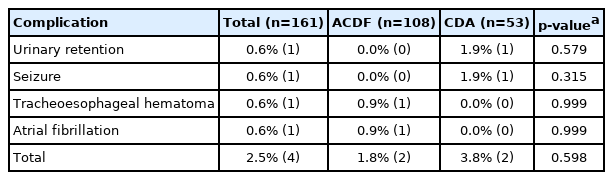
Demographic information (Table 1) regarding a patient’s age, gender, body mass index (BMI), tobacco use, diabetic status, and insurance collected were recorded prior to surgery. Additionally, patient fitness for surgery and comorbidity burden were recorded as the American Society of Anesthesiologists physical classification and Charlson Comorbidity Index. Perioperative characteristics were also recorded (Table 2), which included preoperative spinal pathology, number of operative levels, operative level, use of an anterior cervical plate or stand alone interbody cage, operative duration (from first skin incision to final closure), estimated intraoperative blood loss (EBL), length of postoperative stay (LOS), and day of discharge. Each incidence of a postoperative complication was recorded, reviewed, and summarized (Table 3).
3. Patient Reported Outcomes
The primary outcome of interest of this study was dysphagia scores as evaluated by the SWAL-QOL survey, which is a 44-item questionnaire separated into 11 separate domains that assess the impact of swallowing difficulty on a patient’s quality of life [17]. The individual domains include: dysphagia burden, eating duration, eating desire, symptom frequency, food selection, communication, fear, mental health, social, fatigue, and sleep. Each domain has a variable number of questions, which assess the severity of dysphagia’s impact. All 11 domains are equally weighted to produce a total SWAL-QOL score (out of 100) where a lower score indicates worse symptoms of dysphagia and a higher score implies more favorable symptoms.
In addition to the SWAL-QOL questionnaire, patient neck and arm pain as well as neck disability due to pain were also evaluated using the Visual Analogue Scale (VAS) and Neck Disability Index (NDI). VAS is a continuous pain rating scale with higher values indicating worse pain. NDI is a survey adapted from Oswestry’s Disability Index and evaluates severity of dysfunction due to pain across 10 different domains. Like SWAL-QOL, each domain equally contributes to an overall score (NDI=Total Score/Total Potential Score). A higher NDI score indicates worse disability. All PROMs were administered at preoperative and postoperative (6 weeks, 12-weeks, 6-months) timepoints using an Outcomes Based Electronic Research Database (OBERD, Columbia, MO) through a private patient portal.
4. Statistical Analysis
Prior to statistical analysis, patients were separated into groups according to which cervical procedure they underwent (ACDF vs. CDA). Differences in demographics and perioperative characteristics were evaluated using either a Student’s t-test for continuous values or a chi-square test for categorical variables. Prevalence of postoperative complications were evaluated for differences between the two groups using a chi-square test. Differences in mean PROM scores between groups were evaluated using an unpaired Student’s t-test. An unpaired Student’s t-test was also used to evaluate intergroup differences at each timepoint for individual SWAL-QOL domain scores. A sub-analysis was also performed whereby the ACDF group was further sub-categorized according to use of an anterior cervical plate. Differences in mean overall PROM scores as well as the individual domains at each timepoint was then evaluated using an analysis of variance (ANOVA) and post-hoc Tukey test. Simple regression analysis was utilized to evaluate whether the number of fusion levels operated on were significantly associated with postoperative outcomes. All statistical tests were performed using StataIC (StataCorp LLC, College Station, TX) and had the ɑ value set to 0.050 to reject the null hypothesis.
RESULTS
1. Study Cohort
An initial 312 patients were identified as eligible for this study and after inclusion and exclusion criteria were applied the final study cohort was 161 patients. Patients had a mean age of 47.5 years and mean BMI of 29.5 kg/m2 with a majority being male (62.7%). A higher proportion of diabetics was observed in the ACDF group (p=0.009) and also had a higher mean CCI (1.2 vs. 0.5; p=0.012) (Table 1). The most prevalent preoperative spinal pathology was herniated nucleus pulposus (91.3%) and 86.2% of patients reported clinical symptoms in line with myeloradiculopathy. Majority of procedures were performed at a single level (62.1%) with the most common 1-level procedure performed at C5-6 (28.6%) and 2-level procedures at C5-7 (29.2%). The ACDF group had a significantly longer operative duration (p=0.025) (Table 2). A total of 4 postoperative complications were recorded: 1 patient had urinary retention, 1 patient has a seizure, 1 patient had a tracheoesophageal hematoma, and 1 patient with a history of paroxysmal atrial fibrillation experienced atrial fibrillation (Table 3).
2. Patient Reported Outcomes
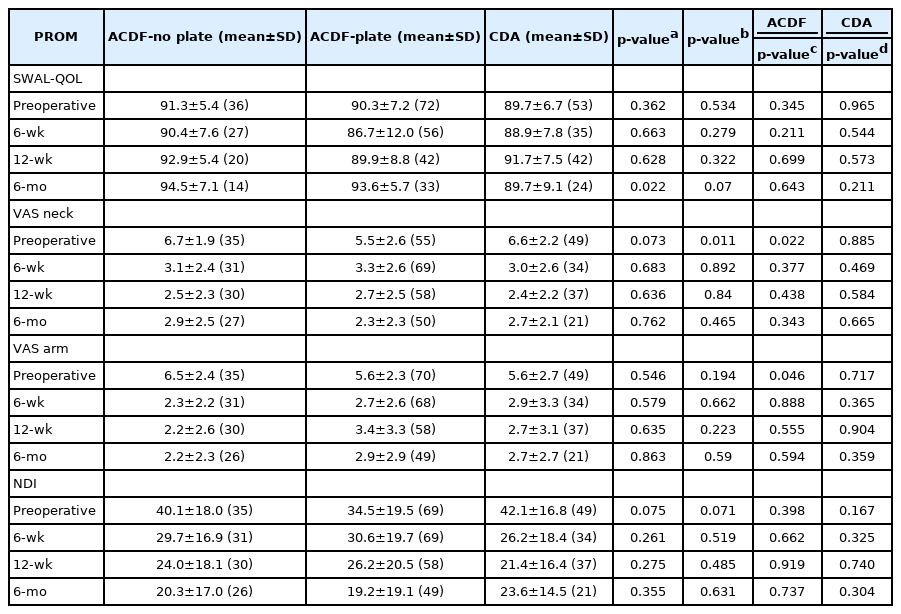
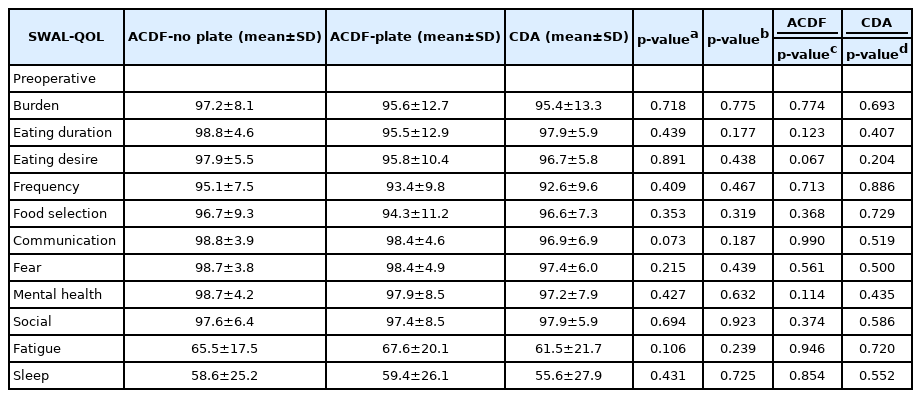
At the preoperative timepoint, patients who underwent an ACDF procedure with use of a stand alone cage reported a SWAL-QOL score of 91.3±5.4. Patients who underwent an ACDF with use of an anterior cervical plate recorded a preoperative score of 90.3±7.2 and those who underwent a CDA had a score of 89.7±6.7. No significant differences in SWAL-QOL between all groups were demonstrated (p=0.362; p=0.534) (Table 4). Group and subgroup analysis also demonstrated no significant differences in preoperative VAS arm and NDI scores (p≥0.071, all); however, testing of subgroups revealed significant differences for VAS neck (p=0.011) (Table 4). Post-hoc testing demonstrated significant differences in mean preoperative VAS neck between ACDF-No plate and ACDF-Plate individuals (6.7±1.9 vs. 5.5±2.6) and ACDF-Plate and CDA (6.6±2.2 vs. 5.5±2.6). Postoperatively, no significant differences in dysphagia scores between groups were demonstrated except for at 6-months where CDA patients had a worse score compared to ACDF patients (p=0.022). No significant associations were found by linear regression analysis between the number of levels operated on and postoperative PROMs (Table 4).
3. SWAL-QOL Domains
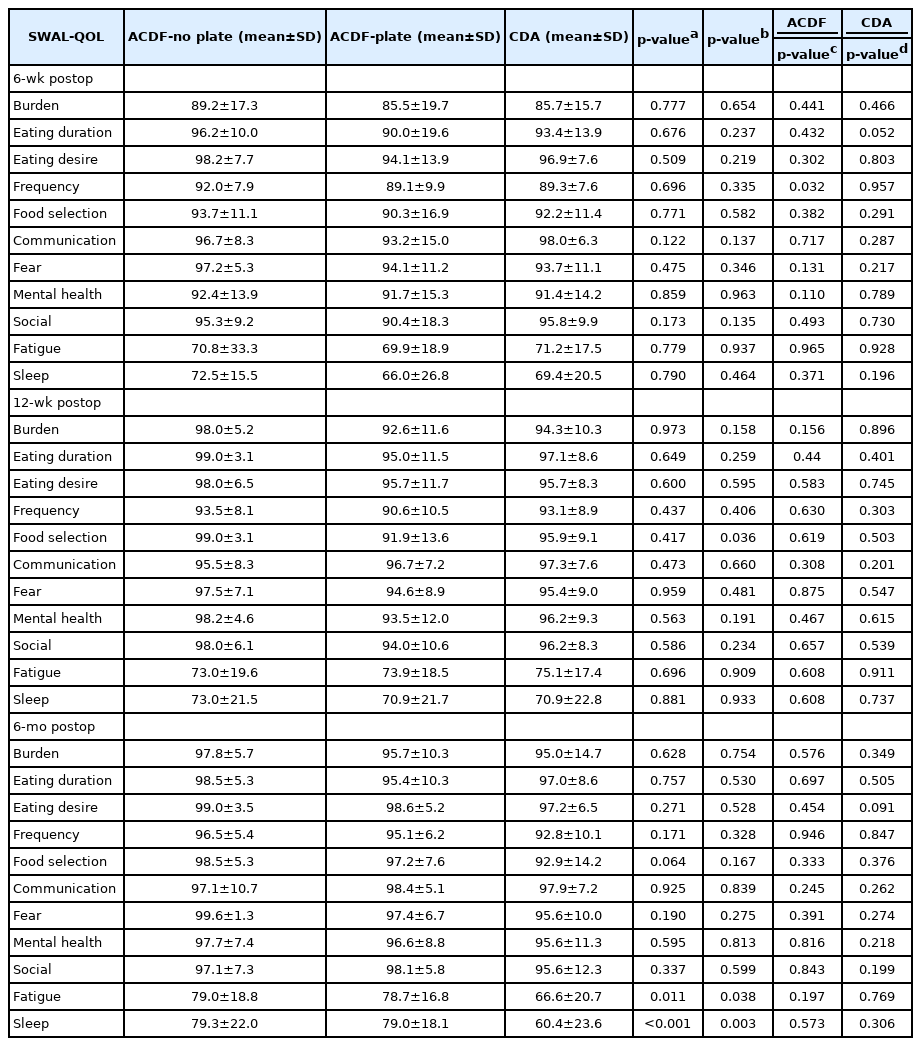
Evaluation of score for each domain demonstrated no significant differences at the preoperative timepoint both when comparing groups and subgroups (p≥0.073, all) (Table 5). At 6 weeks follow-up, ACDF and CDA patients again did not demonstrate any significant differences in any of the SWAL-QOL domains. However, at the 12 week timepoint ACDF patients demonstrated a significant difference in scores for the “food selection” domain with patients receiving an anterior cervical plate reporting a worse value (p=0.036) (Table 6). At the 6-month timepoint, ACDF patients reported a significantly better score for both “Fatigue” and “Sleep” domains. Further subgroup analysis demonstrated that both ACDF subgroups (plate and stand alone cage) demonstrated significantly better “Fatigue” scores compared to the CDA group (p≤0.038). A similar observation was noted for the “Sleep” domain with again both group and subgroup analysis demonstrating a better score with ACDF patients compared to CDA patients (p<0.001; p≤0.003) (Table 6). None of the SWAL-QOL domains were significantly associated with number of fusion levels, other than symptom frequency at 6-weeks following ACDF (p=0.032) (Table 6).
DISCUSSION
Anterior cervical spine surgery is a highly effective treatment for intractable neck pain and disability [27]. One of the most common complications linked to these operations is oropharyngeal dysphagia [28], which has been previously assessed in ACDF and CDA populations subjectively using the Bazaz Scale, MD Anderson Dysphagia Inventory, the Hospital for Special Surgery Dysphagia and Dysphonia Inventory, and the Dysphagia Short Questionnaire [7,18,20]. However, few studies have evaluated swallowing difficulty using the SWAL-QOL questionnaire, and even fewer have longitudinally compared this outcome measure in cervical fusion versus arthroplasty patients [17,22,29-31]. Thus, after assessing SWAL-QOL in CDA and ACDF patients, this study reports similar overall outcome scores between groups with longitudinal differences in fatigue and sleep in relation to dysphagia.
After initial analysis of patient demographics and perioperative characteristics, significant differences were found in diabetes status, CCI score, and operative time between procedure groups. However, these variances likely did not affect long term postoperative dysphagia occurrence, as previous literature does not report CCI score or diabetes as risk factors [32,33]. In the present study, a significantly shorter operative time was seen for CDA than ACDF procedures, which is in contrast to previous literature reporting either longer operative time for CDA as compared to ACDF or no differences in duration of surgery [4,34]. This may be explained by the fact that our ACDF cohort included a larger proportion of patients who underwent plate placement, which has been previously shown to induce longer operative times than the stand alone cage method [35]. Additionally, procedure duration in orthopaedic surgeries is itself dependent on factors such as physician experience and hospital workflow as well [36]. Regardless, it is unlikely that this difference in operative time solely influenced dysphagia scores in the long-term periods evaluated in this study, as any potential effects have previously been shown only in the immediate postoperative days 1 and 2 [37].
In addition to these baseline characteristics, this study also considered improvement of clinical outcomes such as pain and disability. Preoperatively, VAS neck pain scores were significantly poorer for the CDA group than ACDF patients. This is possibly related to the fact that a greater percentage of CDA patients had an initial pathology of myeloradiculopathy, which may induce more severe pain in the afflicted due to compression of both the nerve roots and spinal canal [38]. However, this cannot be concluded with certainty as severity of symptoms and its relationship with radiographic findings was not assessed. Postoperatively, no significant differences between groups for the VAS neck, VAS arm, and NDI scores were found at any time points. Many investigations comparing ACDF and CDA have reported similar quality of life outcomes through long term follow ups of 2 years [39-41]. A few studies do report, though, that NDI and neck pain scores may be statistically better in those undergoing CDA rather than ACDF [42,43]. These differences may arise as a result of an inherent advantage of the CDA surgery, in that it allows patients to have a better postoperative range of motion than what is experienced after cervical fusion [34]. With range of motion preserved, these patients may be able to experience improvements in disability and neck pain to a greater extent.
Along with analysis of the former postoperative outcomes, dysphagia was quantified through SWAL-QOL scores at all timepoints. Overall, there were no differences between the ACDF and CDA groups in dysphagia outcomes, other than at the 6 month time point where CDA patients reported significantly poorer scores than ACDF patients. Interestingly, prior studies using other dysphagia assessment tools have reported lower incidences of postoperative dysphagia over the 1 to 2 years following CDA versus ACDF [44,45]. Although, our findings may be supported by McAfee et al. [46] who reported an increase in dysphagia in 42% of arthroplasty patients at the 3 month time point before eventual resolution at 1 year. Perhaps these fluctuating incidences are due to the transient nature of the condition itself, as dysphagia may newly arise at any point in the postoperative period. For example, swallowing difficulty may occur immediately after operation or even more than a month following anterior cervical spine surgery [28]. Future studies may provide further clarification of this complication’s progression by continuing to track SWAL-QOL scores further out to 1 or 2 years postoperatively. Another factor that may have influenced this finding is the low number of patients in the CDA group who completed the SWAL-QOL questionnaire up to 6 months. As such, patients with extremely low scores may have a greater effect on the overall score for the group at this time point, which is reflected by the high standard deviation as well.
Dysphagia incidence was analyzed further through specific domains in the SWAL-QOL survey, which represents various aspects of daily life, and significant differences were observed at 12 weeks and 6 months. In the Food Selection domain, the ACDF no plate group had higher scores than the anterior plate group at 12 weeks. As previously reported in literature, this may be a result of the reports that suggest ACDF performed with a stand alone cage is superior in reducing dysphagia related complications at earlier time points than the ACDF with an anterior plate method [47,48]. With less difficulty in swallowing, patients may be able to be more liberal in selecting which foods to intake. However, other studies have conversely demonstrated that dysphagia was not significantly different between ACDF with and without plate groups [24,35,49]. Though, due to the fact that only one of these studies utilized SWAL-QOL as an assessment tool, further evaluation with larger ACDF cohorts using this psychometric tool are required for greater elucidation of differences within this domain. Better comprehension of the effects on this attribute of a patient’s quality of life can help enhance the guidance provided to individuals during their recovery period.
Cervical spine patients also presented with different mean values for fatigue and sleep domains, both with lower scores in the CDA group, at the 6 month follow up. Additionally, these patients also had poorer baseline scores in those two domains as well and, as a result, may have required a greater magnitude of dysphagia improvement to ameliorate their fatigue and sleep. It is possible that this trend is related to overall swallowing difficulty as CDA patients also reported worse overall SWAL-QOL scores at 6 months. A previous study also indicated that patients who underwent CDA had higher rates of persistent postoperative neck pain than ACDF patients at 9 months post op [50]. It is plausible that given the CDA group also reported initially higher VAS neck pain scores, some residual neck pain may have had adverse implications on sleep and fatigue. Further investigations must specifically consider the interplay of dysphagia or pain with sleep and fatigue in CDA versus ACDF patient populations.
ACDF and CDA are both generally effective surgical treatments in terms of overall improvements in postoperative quality of life outcomes including dysphagia. However, specific aspects of life such as sleep and fatigue related to swallowing issues may be experienced differently by those undergoing CDA procedures at long term timepoints. The present study adds to the existing literature on the safety and efficacy of utilizing CDA as a result of comparable clinical outcomes to ACDF. To the author’s knowledge, this study is among the first to provide greater information on the utility of the SWAL-QOL questionnaire for evaluation of not only dysphagia but also of particular aspects of quality of life related to this complication for two types of cervical spine surgeries. Physicians may then have greater information to consider incorporating SWAL-QOL, in whole or abridged [22], into their preoperative and postoperative assessment of cervical spine candidates for either arthroplasty or fusion surgery. Through evaluations with this survey, clinicians can provide more detailed preoperative patient education on possible dysphagia occurrence and any repercussions on patients’ daily lives.
Limitations
There are a few limitations to the present study that must be considered. The study’s design itself lends to possible observer and selection bias, as is the case with any retrospective investigation. Additionally, a level of responder or recall bias for long term timepoints may be present, as self reported surveys were utilized to assess postoperative outcomes. Given the lengthy nature of the questionnaire, this study was also limited by diminishing patient compliance further into the postoperative period. This in turn may restrict our ability to determine the longitudinal impact of dysphagia within the two surgical populations. Potentially the implementation of an abridge yet valid SWAL-QOL may adequately serve the same purpose while not jeopardize the quality of information collected [22]. Though dysphagia was not clinically assessed and diagnosed, subjective measures such as patient surveys may be more amenable to accurately evaluating sensations of swallowing difficulty. Furthermore, since sleep and fatigue SWAL-QOL scales measure general quality of health and are not dysphagia-specific, confounding variables such as patient comorbidities may have provided significant bias. It is worthwhile mentioning that patients with single- and double-level procedures were included, which may introduce clinical heterogeneity and data bias. We addressed this limitation by performing simple regression analysis, which demonstrated no significant relationship between postoperative outcomes and number of levels operated on, other than for symptom frequency at 6-weeks following ACDF. Moreover, all patients in our cohort underwent surgery at a single institution with one surgeon, which may limit the applicability of our results to larger, general populations. Future comparative studies should include multiple surgeons in multicentered settings to strengthen the results of this study.
CONCLUSION
Postoperative outcomes of pain, disability, and dysphagia were generally similar between patients undergoing ACDF or CDA procedures. At long term follow ups, poorer fatigue and sleep as measured by the SWAL-QOL questionnaire domains were reported by CDA patients in comparison to those undergoing ACDF. Although quality of life outcomes are generally comparable between CDA and ACDF patients, those who undergo cervical disc arthroplasty may experience worse fatigue and sleep possibly in relation to dysphagia at longitudinal timepoints.
Notes
No potential conflict of interest relevant to this article.