INTRODUCTION
Lumbar juxtafacet cysts (JFCs) include both synovial and ganglion cysts located adjacent to the facet joint or arising from the ligamentum flavum [1,2]. Lumbar JFCs may cause symptomatic nerve root and thecal sac compression, leading to radiculopathy, neurogenic claudication, and back pain [1,3]. Surgical treatment should be considered if refractory pain persists despite conservative management. The surgical approaches for these lesions have evolved from open surgery to minimally invasive methods, such as the Wiltse approach using a tubular retractor and uniportal or biportal endoscopic approach [4-7]. Moreover, interlaminar contralateral approaches using a microsurgical tubular retractor system or endoscopic systems can preserve the facet joint during the resection of lumbar JFC [4,8,9]. These advanced surgical approaches are usually used to treat lumbar intraspinal JFC and lumbar foraminal JFC.
Extraforaminal JFCs are rare and present a surgical challenge due to its anatomical location. In previously reported cases, a microscopic paraspinal approach was mainly used to resect the extraforaminal cysts at the L5-S1 level with total or partial facet joint removal [10,11]. Recently, Telfeian et al. [12] described a full endoscopic transforaminal approach to resect a lumbar extraforaminal JFC.
Uniportal interlaminar contralateral endoscopic lumbar foraminotomy (ICELF) has the optimized benefits of using a small-diameter endoscopic system that can pass through the foraminal space, nearly parallel to the exiting nerve root, making foraminal and extraforaminal nerve root decompression without retraction [13-15]. However, the interlaminar contralateral approach for extraforaminal cysts has not been reported.
This study aimed to introduce the surgical technique of ICELF for extraforaminal juxtafacet cyst removal and reveal its approach-related benefits with operating cases treated by the ICELF technique.
CASE REPORT
Case 1.
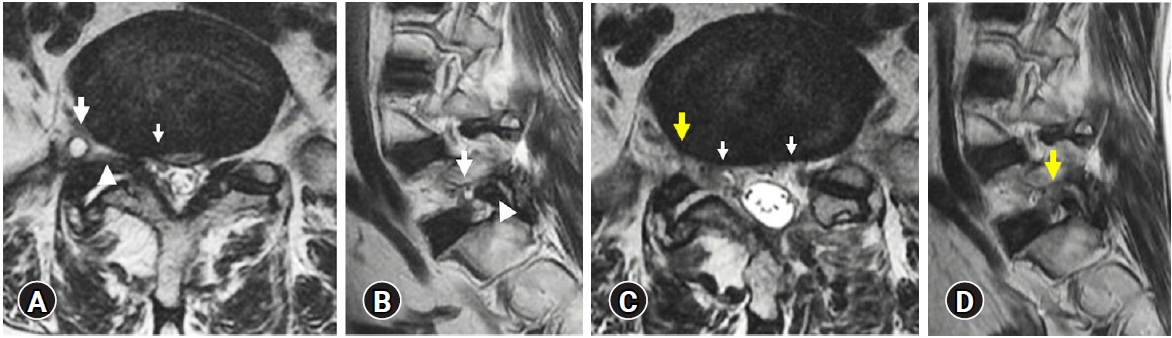
An 83-year-old man presented with a 12-month history of progressively increasing pain in the right lower back, buttock, and right leg. The pain radiated through the right L5 dermatome. The pain increased while standing, walking, and bending to the right. On physical examination, the patient showed hypesthesia of the L5 nerve root distribution in the right leg, however no motor weakness was detected. The straight-leg-raising test and bilateral knee and ankle reflexes were normal. Magnetic resonance imaging (MRI) showed a cyst in the extraforaminal region and foraminal stenosis at the right L5-S1 level. The cyst was in the cranial-dorsal part of the extraforaminal space compressing the exiting nerve root in the caudal direction (Figure 1A, B). Another cyst, which was smaller than the previous one, was observed in the extraforaminal space at the right S1-S2 level on a sagittal MRI scan, and two adjacent cysts at the L5-S1 and S1-S2 levels were connected to the L5-S1 facet joint (Figure 1B,). We performed the ICELF surgery to treat the extraforaminal JFC. Postoperative MRI revealed well decompressed foraminal stenosis and complete resection of the extraforaminal cysts (Figure 1C, D).
Case 2.
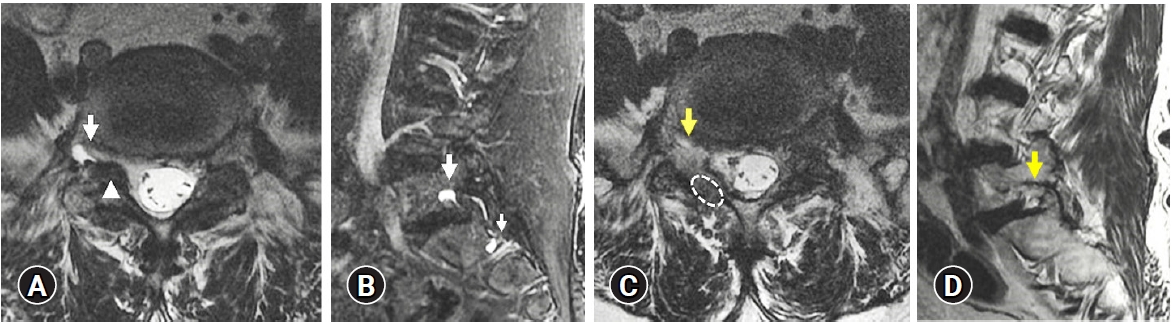
A 62-year-old woman presented with an 8-month history of intractable pain in the right lower buttock and both legs despite conservative treatment at another clinic. The pain radiated through the right L5 dermatome and the S1 dermatome on both the legs, and was aggravated while walking and sitting. On physical examination, the patient showed motor weakness of the right ankle, great toe extension of grade 4 (out of 5), and decreased sensory function of the L5 nerve root distribution in the right leg. The straight-leg-raising test was positive for the right side at 50°. Knee and ankle reflexes were normal. MRI showed a right-sided extraforaminal cyst, facet joint osteoarthritis, foraminal stenosis, and bilateral lateral recess stenosis at the L5-S1 level. The cyst was in the cranial-ventral part of the extraforaminal space compressing the exiting nerve root in the caudal-dorsal direction (Figure 2A, B). Preoperative MRI did not show the connection between the cyst and adjacent facet joint. Conservative treatment with painkillers and physiotherapy was performed for more than 6 months without improvement. Progressive deterioration of the symptoms was the indication for surgery. After ICELF surgery, postoperative MRI showed the entire removal of the extraforaminal cysts (Figure 2C, D). Coexisting foraminal and lateral recess stenosis in the female patient was also adequately decompressed (Figure 2C, D). Pathologic examination of surgical specimen revealed a synovial cyst. Both the patients did not experience any perioperative complications. Radiating pain in the right leg, back pain, leg hypesthesia, and ankle weakness improved. At the 12-month follow-up, both the patients were satisfied with the surgical result without any relapse of symptoms.
SURGICAL PROCEDURES (Video 1)
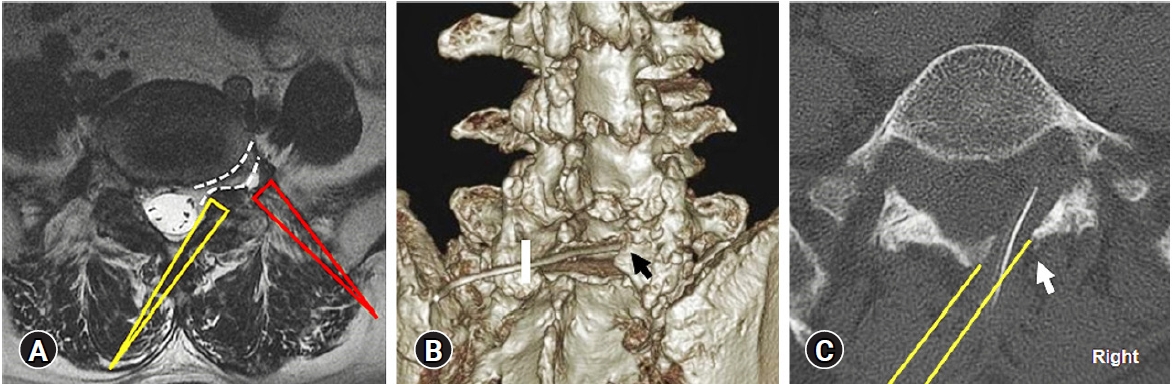
Meticulous dissection between the cyst and nerve root and visualization of the entire cyst contour are critical for safe and complete removal of the cyst adhered to the nerve root. Therefore, we used ICELF to remove the extraforaminal cystic lesion according to the method described by Kim et al. [13,14] and Wu et al. [15]. The endoscopic system used in this technique passes through the foramen along the exiting nerve root offering a direct endoscopic view of the area from the caudal-dorsal part of the foramen to cranial-ventrally located cyst and the site of cyst-nerve root adhesion (Figure 3A).
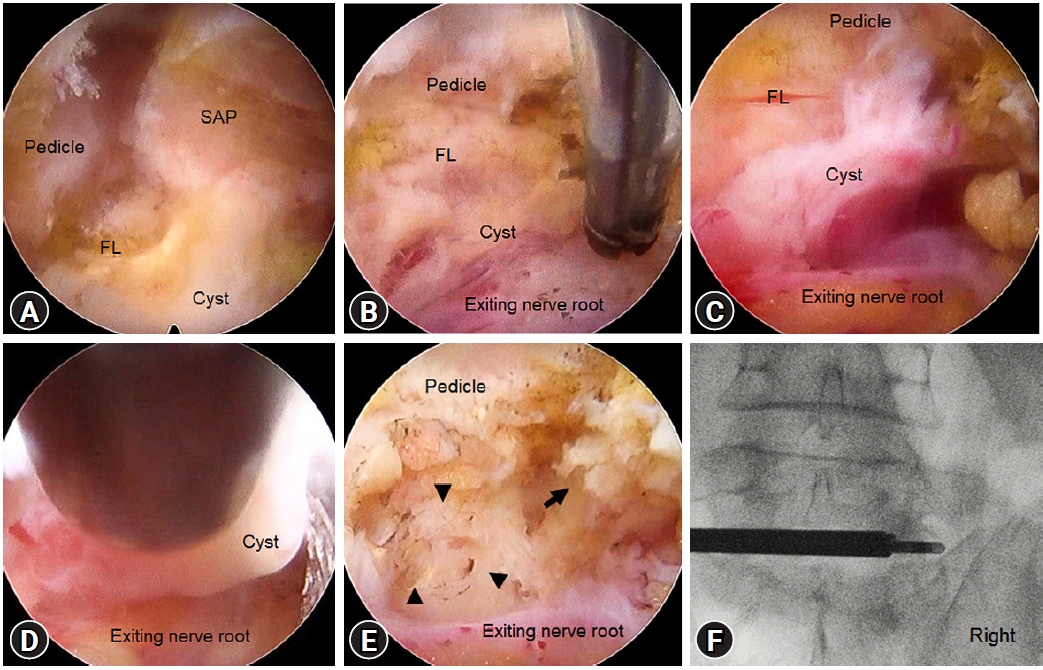
We used an endoscope with a viewing angle of 30°, outer diameter of 7.3 mm, 4.7-mm working channel, and a total length of 251 mm. The endoscope was docked on the spinolaminar junction of the ipsilateral side, and contralateral sublaminar drilling was performed to create a sublaminar space up to the contralateral medial part of the foramen (Figure 3B, C). The thickened ligamentum flavum in the medial foraminal region was removed using endoscopic forceps. The foramen was explored with the scope after drilling the overriding superior articular facet and removing the foraminal ligamentum flavum, and the exiting nerve root was then observed. As the foramen was enlarged, the endoscope was introduced deeper through the caudal-ventral part of the foramen to explore the extraforaminal cyst. The endoscope was carefully advanced into the extraforaminal space to avoid violation of the foraminal disc by the beveled working cannula. The cyst was observed between the exiting nerve root and foraminal ligament in the lateral aspect of the neural foramen; it was located cranial-ventrally to the L5 nerve root, embedded in the foraminal ligament, and severely adhered to the exiting nerve root (Figure 4A, B). The site of cyst-nerve root adhesion was confirmed under direct endoscopic vision, and meticulous dissection was performed using the flexible tip of the radiofrequency-ablation catheter (Figure 4B). The entire cystic wall was safely removed in piecemeal fashion from the attached site on the foraminal ligament and L5 exiting nerve root using the endoscopic forceps. (Figure 4C, D). After complete cyst removal, the nerve root was fully decompressed, and the suspected connection site between the cyst and adjacent facet joint was confirmed in the first case (Figure 4E; however, the connecting site was not found in the second case. Complete decompression was confirmed by an intraoperative X-ray (Figure 4F).
DISCUSSION
Extraforaminal JFCs are rare. In previously reported extraforaminal JFC cases, a microscopic paraspinal approach was mainly used to resect the cysts at the L5-S1 level with total or partial facet joint removal [10,11] because anatomical obstacles, such as narrow surgical corridor due to the large facet joint, prominent L5 transverse process, and iliac bone, limit the approach to reach the extraforaminal cyst. The Wiltse approach is a minimally invasive procedure proposed to remove extraforaminal JFCs, but the tubular retractor docked onto the facet joint may obstruct the visualization of the facet itself [16]. Recently, a transforaminal endoscopic approach with optimized oblique access to obscure pathology was performed to successfully remove lumbar extraforaminal JFCs at the L5-S1 level [12].
Extraforaminal cysts are usually located in the cranial-dorsal aspect of the exiting nerve root [2], and they obscure the exiting nerve root and nerve root adhesion site during the paraspinal Wiltse approach or transforaminal endoscopic approach. In this situation, partial cyst removal may be required to expose the nerve root adhesion site, and meticulous dissection may be difficult due to disruption of the original structure.
The cyst and nerve root adhesion site can be exposed without partial cystectomy during the endoscopic transforaminal approach. However, nerve root retraction using a working cannula may be necessary because the endoscopic system approaches the cyst and nerve root with a steep angle (Figure 1A). Nerve root retraction while the root is in a compressed state may induce neural injury such as postoperative dysesthesia.
In the present report, both the patients had extraforaminal JFC located in an obscured area in the cranial-dorsal and cranial-ventral part of the nerve root, accompanied by symptomatic foraminal stenosis. Nerve root retraction was inevitable during cyst removal with an endoscopic transforaminal approach, and the decompression of symptomatic foraminal stenosis was necessary to resolve the L5 radiculopathy. Under these circumstances, we performed ICELF and obtained successful outcomes due to the several approach-related benefits.
The fine endoscopic system with 7.3 mm outer diameter was advanced from the opening of the medial foramen to the extraforaminal region in parallel with the exiting nerve root without retraction. A 30° oblique surgical view of the exiting nerve root was obtained from the endoscope located at the caudal part of the foramen. Therefore, the cranial-ventrally and cranial-dorsally located JFCs and the site of cyst-nerve root adhesion could be clearly visualized. Then, the meticulous dissection between the cyst and nerve root could be performed, and the entire cyst capsule was removed; these minimally invasive procedures might prevent neural injury and cyst recurrence.
The origin of the cyst was explored from the medial foraminal part to the extraforaminal part of the facet joint along the exiting nerve root; the facet joint connection was found in one patient, whereas it was not observed in the other patient under an endoscopic view. However, on pathologic examination, surgical specimens from both the patients were confirmed to be synovial cysts. These findings support the hypothesis that all JFCs, located in both usual and unusual locations, are derived from the facet joint [2].
The present case report may have significant scholarly information and operative technical importance for the following reasons. First, this is the first report of a cyst severely adhered to the nerve root, and the structure of its origin was confirmed without partial cystectomy under a direct endoscopic view. Second, this is the first case in which the entire cysts were successfully removed using ICELF. Third, the entire cyst was safely removed without nerve root retraction, even in the presence of foraminal stenosis. Finally, symptomatic foraminal stenosis was also resolved with minimal drilling of the medial facet joint and without violating the intervertebral disc.
There are several points to consider before performing ICELF for extraforaminal JFC. ICELF requires skillful instrument handling in the narrowed lumbar foraminal space; therefore, surgeons accustomed to endoscopic intraspinal and transforaminal surgery may successfully perform this procedure. ICELF is suitable for resolving double-exiting nerve compressions due to the extraforaminal cyst with coexisting symptomatic foraminal stenosis with one surgical approach. The full endoscopic transforaminal or biportal endoscopic paraspinal approach may be more efficient for extraforaminal cyst removal and not for resolving double crushed lesions. Furthermore, if the extraforaminal cyst is suspected to originate from the medial facet joint on MRI, ICELF is recommended because the entire cystic contour and the site of cyst’s origin can be detected efficiently in this procedure, enabling the complete removal of cystic wall.
CONCLUSION
ICELF for the treatment of extraforaminal JFC can be an alternative surgical method to resolve symptomatic foraminal stenosis and the cyst simultaneously. The endoscopic system moves parallel to the exiting nerve root during ICELF, facilitating clear visualization of the cranial-dorsally or cranial-ventrally located extraforaminal JFCs. The entire cyst contour and the site of cyst-nerve root adhesion can be detected without nerve root retraction, and meticulous dissection is possible without violating the cystic wall.