AbstractObjectiveThe aim of this study was to describe the surgical techniques and preliminary results of inside-out biportal endoscopic posterior cervical foraminotomy (BEPCF) for unilateral cervical radiculopathy.
MethodsThis study involved 36 consecutive patients (38 segments) who underwent BEPCF for unilateral cervical radiculopathy between November 2020 and June 2022. Foraminotomy was performed using the biportal endoscopic technique, with the surgeon standing on the opposite side and making skin incisions on the same side of the foramen stenosis. After widening of the V-point and exposing the nerve root using a high-speed drill, we used a curved osteotome to undercut the facet joint from inside the foramen to complete the nerve root decompression.
ResultsThe study followed patients for an average of 15.5 months and found significant improvements in the visual analog scale for arm pain, from 7.3±2.2 to 0.9±0.7 (P<0.005), and the Neck Disability Index, from 54.6±16.9 to 14.6±12.6 (P<0.005). Almost all patients (94.4%) had good or excellent results. Hospitalization lasted an average of 3.2 days and postoperative magnetic resonance imaging showed successful neural decompression. Complications were minimal, with only two cases of asymptomatic root abrasions and one case of transient neuralgia. One patient required re-operation due to incomplete decompression.
INTRODUCTIONCervical radiculopathy typically presents with neck pain, arm pain, paresthesia, numbness, or motor weakness due to inflammation or compression of the cervical nerve root [1,2]. The most common causes of cervical radiculopathy are cervical disc herniation and cervical spondylosis [3,4]. While anterior cervical discectomy and fusion (ACDF) has been considered the gold standard in managing cervical radiculopathy [5], the literature shows a variety of complications associated with the procedure, including adjacent segmental diseases, pseudoarthrosis, postoperative dysphagia, vascular injury, recurrent laryngeal nerve palsy, cerebrospinal fluid leakage, and hematoma [6-8].
Traditional posterior cervical foraminotomy (PCF) was developed long before ACDF and is recognized as a simple and effective surgical treatment for cervical radiculopathy [9]. It avoids the complication associated with anterior approach and preserves the mobility of the operated segment [9-11]. However, traditional PCF requires a large surgical incision and massive dissection of the posterior neck musculo-ligamentous structures. The extensive soft tissue damage resulting from this approach may lead to severe wound pain, delayed recovery, and a high incidence of postoperative neck pain [9,12,13]. In addition, excessive facet joint destruction may lead to the concerns for post-decompression segmental instability which requires a second operation for reconstruction [14,15].
In recent years, spine surgeons have paid attention to the biportal endoscopic technique. This technique is performed through two independent portals with continuous irrigation of normal saline, providing hydrostatic pressure to suppress bleeding and carry away bone debris and oozing. Combined with a high-resolution endoscope, the biportal endoscopic technique provides a clear, bright, and magnified surgical field of view, enabling surgeons to perform delicate surgical procedures without excessive soft tissue damage. This minimally invasive technique has been applied to address a variety of spinal pathologies, such as discectomy for lumbar disc herniation, laminotomy for degenerative lumbar spinal stenosis, and lumbar interbody fusion for disc degeneration or spondylolisthesis, all of which have demonstrated good clinical efficacy [16-21].
Recently, we have performed biportal endoscopic posterior cervical foraminotomy (BEPCF) in patients with unilateral cervical radiculopathy, attempting to make traditional PCF a minimally invasive procedure. The purposes of the study are to describe the surgical techniques in detail, and to evaluate the preliminary clinical outcomes.
MATERIALS AND METHODS1. Patient SelectionThis case series included 36 consecutive patients who received 38 segments of biportal endoscopic posterior cervical foraminotomy (BEPCF) between November 2020 and June 2022. The patients were 24 males and 12 females with an average age of 56.8 years (range 39–63 years).
Indications for BEPCF were radicular arm pain, single or multiple cervical radiculopathies due to foraminal stenosis, with persistent symptoms for more than three months and failure of conservative treatment. We excluded patients with segmental instability, kyphotic sagittal alignment, and prior surgeries in their cervical spines. Patients with central canal stenosis and myelopathy, characterized by abnormally increased deep tendon reflexes, hyperclonus of ankles, abnormal Babinski reflexes, or gait disturbance were also excluded. Thirty-four patients received one-segment decompression, while two patients received two-segment decompression (Table 1). All surgeries were performed by the senior author in a single medical center.
2. Evaluation of Clinical Data and OutcomesWe obtained demographic and clinical data, as well as treatment outcomes, through chart reviews. All patients underwent baseline evaluation before surgery, followed by evaluations at 1 month, 3 months, 6 months, and 1 year after surgery, and then annually thereafter. Outcome measures included the visual analog scale (VAS) for arm pain, the neck disability index (NDI) for disability [22], and the modified MacNab criteria for the overall outcomes [23].
All patients underwent plain X-rays of AP, lateral, oblique, and dynamic lateral views before the surgery, as well as at 3 months, 6 months, and 1 year after the surgery. Additionally, all patients received a cervical spine magnetic resonance imaging (MRI) study prior to the surgery. The MRI study included T1-weighted and T2-weighted images with 3mm thin slices at sagittal, axial, coronal, and oblique sagittal planes perpendicular to the neuroforamen for evaluation. Post-operative MRI studies were performed at 3 months after the surgery. To evaluate facet preservation, we compared the pre-operative and post-operative axial MRI images using the method described by Matsumura et al. [24] and Dohzono et al. [25]. However, MRI was used instead of CT scan.
The independent t-test was used to compare continuous variables between groups, while the chi-square test was used to compare categorical variables. A p-value of <0.05 was considered statistically significant.
3. Surgical TechniquesBEPCF is performed under endotracheal general anesthesia with the patient placed in a prone position on a radiolucent surgical table with his/her head supported by the headrest. The table must be adjusted to ensure free passage of the fluoroscope to obtain clear anteroposterior and lateral images. The patient’s shoulders are retracted caudally and fixed on the surgical table using adhesive tapes. The table can be tilted head-up or head-down to keep the segment of interest perpendicular to the floor for precise localization and more ergonomic handling of the endoscope and surgical instruments (Figure 1). Since the surgery is performed with continuous saline irrigation, a watertight draping is essential to prevent soaking and resultant hypothermia of the patient.
First, we determine the disc level of interest using the lateral fluoroscopic image. Then, using the anteroposterior images, we draw the skin markings. The V-point (junction of cranial and caudal laminae) must be clearly identified as the initial target for landing the endoscope and surgical instruments. For the contralateral inside-out approach, taking the left side foraminotomy for example, the surgeon stands on the patient’s right side, and the skin incisions are along the left lateral border of the spinous processes, separated by about 2 cm (Figure 2). For a two-segment decompression, a wider separation is needed.
We prefer transverse skin incisions for better cosmetic results. The deep neck fascia is tough and requires a sharp No. 11 scalpel for penetration. Then, we use a blunt dilator to palpate the margins of the laminae around the V-point. The endoscope (4 mm ×30°; ConMed, Largo, Florida) and radiofrequency wand (ArthroCare, Austin, Texas) are inserted through independent skin incisions with inflow of normal saline. The triangulation formed by the endoscope, V-point, and radiofrequency wand must be confirmed under the fluoroscope (Figure 2). Use the radiofrequency wand to ablate the soft tissue to identify the V-point and create the working space required for the following procedures (Figure 3). Good control of saline inflow/outflow is mandatory to maintain a clear surgical field while using the high-speed drilling system.
Starting from the V-point, extend the foraminotomy cranially, caudally, and laterally until the margin of the ligamentum flavum is exposed (Figure 4). A high-speed drill with a 3-mm coarse diamond ball tip (Primado II; NSK, Tokyo, Japan) is used as the primary instrument for removing bone. Use the nerve hook to elevate the ligamentum flavum and the underlying perineural membrane, removing only the portion of the ligamentum flavum which covers the nerve root. Coagulate the bleeders on the perineural membrane or epidural vessels using a 0.8 mm radiofrequency wand, and identify the nerve root. Use a 3-mm wide curved osteotome to undercut the cranial and caudal laminae to identify the inner surface of the pedicles. Then, use the same osteotome to undercut the superior articular process of the caudal vertebra (Figure 5). Use a small, angled curette to remove the bony fragments and free the nerve root. Check the adequacy of decompression and mobility of the nerve root using a nerve hook (Figure 6). Temporarily stop the irrigation to check the pulsation of the nerve root and identify the active bleeders. Use the radiofrequency wand to coagulate the bleeders and bone wax to seal the cancellous bone. Close the wounds by layers, using absorbable sutures to close the skin incisions and adhesive gel to secure them.
To control wound pain, the patient is given oral acetaminophen and intravenous morphine. They are allowed to ambulate with a soft neck collar. Typically, the patient is discharged from the hospital on the second postoperative day.
RESULTSThe average follow-up period was 15.5 months, ranging from 6 to 31 months. The average duration of hospitalization was 3.2±1.2 days, ranging from 2 to 6 days. The mean operation time was 58.4±15.4 minutes per segment of decompression (Table 1). Most patients experienced minimal pain at the surgical sites, and pain control with oral acetaminophen was usually sufficient. Only a few patients required one or two doses of morphine infusion. At the final follow-up, the VAS score for arm pain significantly improved from 7.3±2.2 to 0.9±0.7. The NDI also improved from 54.6±16.9 to 14.6±12.6. All these improvements were statistically significant from the baseline with p<0.005. According to the modified MacNab criteria, 21 patients (58.3%) had excellent results, 13 patients (36.1%) had good results, 2 patients (5.6%) had fair results, and no patient had poor results. The ratio of good and excellent results was 94.4% (Table 2).
All patients underwent regular X-ray evaluations at 3, 6, and 12 months after surgery. We did not observe post-decompression segmental instability in any of our patients. Post-operative MRI follow-up at 3 months after surgery showed adequate decompression and enlargement of the neural foramen at the oblique sagittal plane with minimal facet joint destruction and soft tissue injury (Figure 7, 8). Post-operative MRI data were available for 22 patients, and the average facet preservation rate was 81.7%±8.0%, ranging from 64.5% to 91.5% (Figure 9).
Complications included two asymptomatic root abrasions and one case of transient neuralgia. There were no cases of dural tear or neurological complications. In the very early series, one patient experienced persistent radicular symptoms due to incomplete decompression. To alleviate his symptoms, a revision BEPCF procedure was performed (Table 1).
DISCUSSIONThis study presents a minimally invasive surgical technique for treating cervical radiculopathy using the biportal endoscopic technique. The treatment resulted in good clinical outcomes, including significant improvement in VAS score and ODI, a short hospital stay, and a low complication rate. The contralateral inside-out approach provides adequate nerve root decompression with minimal facet joint destruction and soft tissue injury, while also offering ergonomic settings for the surgeon to perform the surgery.
The estimated annual incidence of cervical radiculopathy is 85 out of 100,000 people, and it usually occurs at the C5/6 and C6/7 levels [2,3]. The most common clinical presentations are radicular arm pain, followed by sensory deficit, neck pain, and reflex deficit [26]. Non-operative management, including medication, programmed rehabilitation, and epidural steroid injection, has been proven to achieve significant symptom relief in 75% to 90% of these patients [3,27]. However, for those who experience intolerable and persistent symptoms after conservative treatment, surgical decompression may be a good alternative solution. There are two mainstreams of surgical treatment: ACDF from an anterior approach, and PCF from a posterior approach [5,28].
ACDF removes the entire disc, restores disc height and lordotic alignment, and reconstructs segmental stability without damaging the posterior neck muscles. It is considered the gold standard surgical treatment for cervical radiculopathy due to its ability to provide quick and effective relief for neck pain, arm pain, and neurological symptoms [5,11,29]. However, there are many disadvantages associated with spinal fusion and the anterior approach that are also well documented in the literature [6-8].
In contrast, PCF decompresses the nerve roots directly via a posterior approach, avoiding the complications associated with an anterior approach. Several studies have shown that PCF provides comparable clinical outcomes in terms of symptom relief, complication rate, and patient satisfaction compared to ACDF, while preserving the range of motion of the cervical spine and avoiding adjacent segment degeneration [3,9,10]. A systematic review conducted by Liu et al. [11] summarizes that there was no significant difference in the complication rate and reoperation rate between ACDF and PCF within 2 years of the initial surgery. A meta-analysis conducted by Fang et al. [5] concludes that PCF is a sufficient alternative to ACDF with shorter operation time, shorter length of hospital stays, and a lower total hospital cost. However, the major drawbacks of traditional PCF are excessive damage to the posterior cervical musculo-ligamentous structures and destruction of the facet joints that contribute to segmental hypermobility and postoperative kyphosis [12,30,31].
To minimize soft tissue damage in open surgeries, a minimally invasive approach using the tubular retractor has been adopted since Dr. Foley and Smith [32] introduced the concept of microendoscopic surgeries in 1997 [33,34]. The microendoscopic PCF shares the advantages of traditional PCF but minimizes iatrogenic damage and has been reported to provide comparable results in clinical outcomes [28,35,36]. However, handling surgical instruments to perform delicate procedures in such a small tubular retractor is challenging. Even with the assistance of a specially designed endoscope or microscope, it still requires a steep learning curve to achieve stable treatment results and reduce the possibility of neurological complications [37].
In this study, we introduce a contralateral inside-out PCF technique using biportal endoscopy to treat cervical radiculopathy. Compared to traditional microscopic or microendoscopic PCF, the biportal endoscopic approach results in an almost bloodless surgical field. Normal saline is used to provide hydrostatic pressure to suppress bleeding and carry away bone debris. Although the working space may be small, a high-resolution 30-degree endoscope provides a clear, bright, wide, and magnified surgical field of view [38-40]. The operator and assistants perform the procedure on a video monitor, eliminating the need to bend their necks or strain their eyes on a microscope. The operator holds the endoscope in one hand and surgical instruments in the other, allowing for a relaxed neck and shoulder posture and minimizing the risk of neurological complications during delicate surgical procedures.
Biportal endoscopic surgery has been successfully used to treat a variety of degenerative conditions in the lumbar spine [16-21]. Several studies have shown that the clinical outcomes of biportal endoscopic surgeries are comparable to those of microscopic or microendoscopic approaches [41-44]. A comparative study of three types of minimally invasive decompressive surgery in patients with lumbar spinal stenosis was conducted by Heo et al. [41]. The study showed that the endoscopy groups, either uniportal or biportal, had better clinical outcomes in the immediate postoperative period than the microscopy group. The better outcomes were possibly due to less soft tissue injury related to surgery in the endoscopy group [41]. Our study also showed that BEPCF is very effective in relieving preoperative arm pain and neurological symptoms, with minimal pain from the surgical sites.
The contralateral inside-out approach differs significantly from the ipsilateral approach (Figure 10). Although the decompression of the nerve root may be equally effective with both approaches, the extent of laminotomy required to achieve an effective decompression is much smaller with the contralateral inside-out approach. Consequently, there is less facet joint destruction. By undercutting the superior articular process, the contralateral inside-out approach may preserve a greater proportion of the facet joint and capsule [45,46]. Therefore, the contralateral inside-out approach may reduce the risk of post-decompression segmental instability or progressive kyphosis after the surgery [14,15]. However, this theoretical advantage requires a long-term follow-up study to validate.
Handling of the endoscope and surgical instruments is more ergonomic for the contralateral inside-out approach. With the surgeon positioned on the contralateral side, the endoscopic viewpoint naturally follows the direction of the nerve root from its origin to beyond the foramen. Additionally, handling surgical instruments aligns with the natural posture of the hand. Conversely, the ipsilateral approach presents the endoscopic viewpoint from the opposite side, forcing the surgeon to handle surgical instruments in a non-ergonomic, reversed manner.
The current study has several limitations. First, it is a retrospective study with a small sample size and short-term follow-up. Second, all surgeries were performed by a single spine surgeon who is experienced in minimally invasive and endoscopic spine surgeries. The treatment results and complications may differ if surgeries are performed by another surgeon with a different level of experience. Third, long-term or comparative studies are needed to verify the theoretical or proposed advantages of the contralateral inside-out BEPCF.
CONCLUSIONBEPCF is a simple, effective, and safe minimally invasive surgical technique for treating unilateral cervical radiculopathy. With appropriate patient selection, spinal fusions and their associated negative consequences can be avoided. When BEPCF is done via the contralateral inside-out approach, the surgeon can perform an effective decompression in an ergonomic setting while preserving the facet joint.
NOTESACKNOWLEDGEMENTSThis study was supported by the Far Eastern Memorial Hospital (grant number: FEMH-2022-C-047).
Fig. 1.Patient positioning. The surgical table is adjusted so that the target disc level is perpendicular to the floor. The result is confirmed using a fluoroscope. 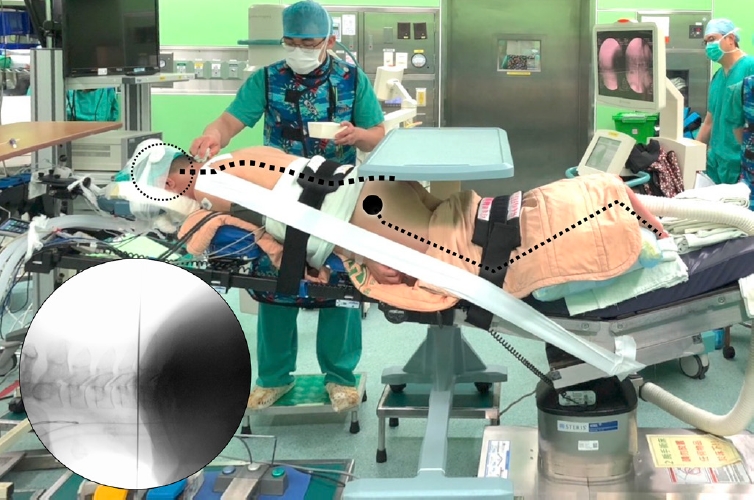
Fig. 2.Skin marking and triangulation. (A) The V-point (red dot) is identified on antero-posterior images. Transverse skin incisions (red lines) should be made along the lateral border of spinous processes, separated by approximately 2 cm. (B) The level and triangulation are confirmed on lateral images. 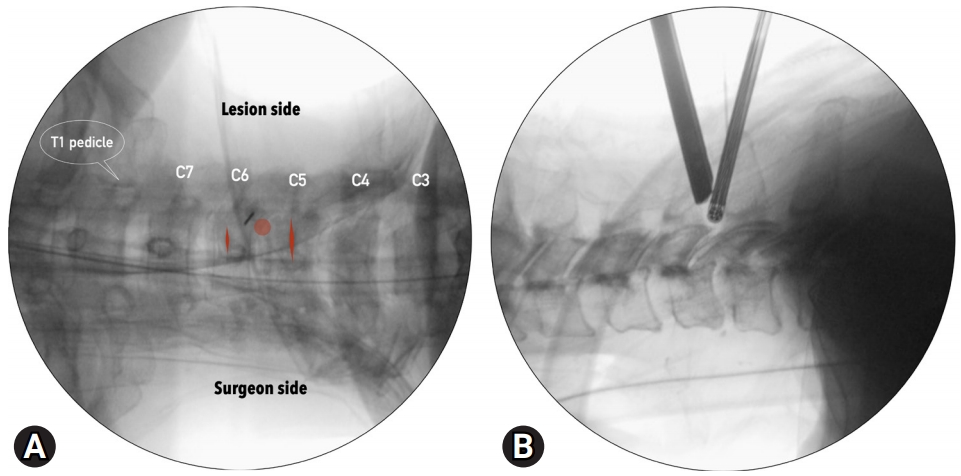
Fig. 3.(A) This illustration demonstrates the foraminal stenosis caused by osteophytes that arise from the uncovertebral joint and hypertrophy of the facet joint. (B) An endoscopic photo shows the V-point viewed in the inside-out approach. 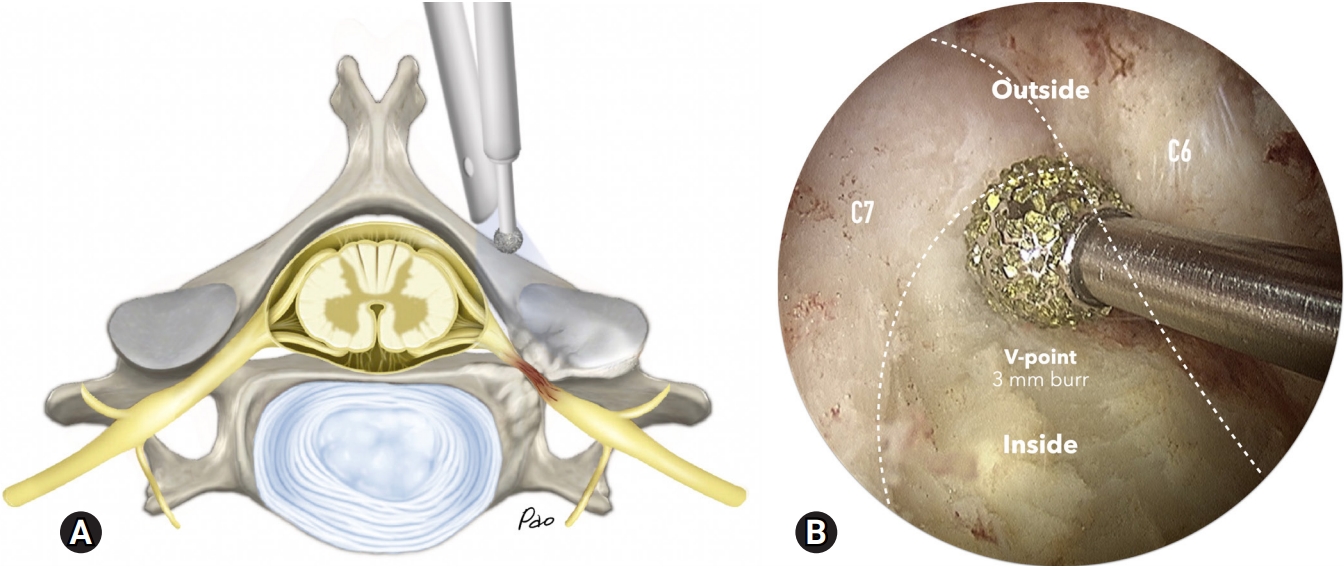
Fig. 4.(A) An illustration demonstrates foraminotomy, which uses a high-speed drill to expose the nerve root. (B) An endoscopic photo shows the facet joint (dashed line) and impingement of the nerve root in the neural foramen. 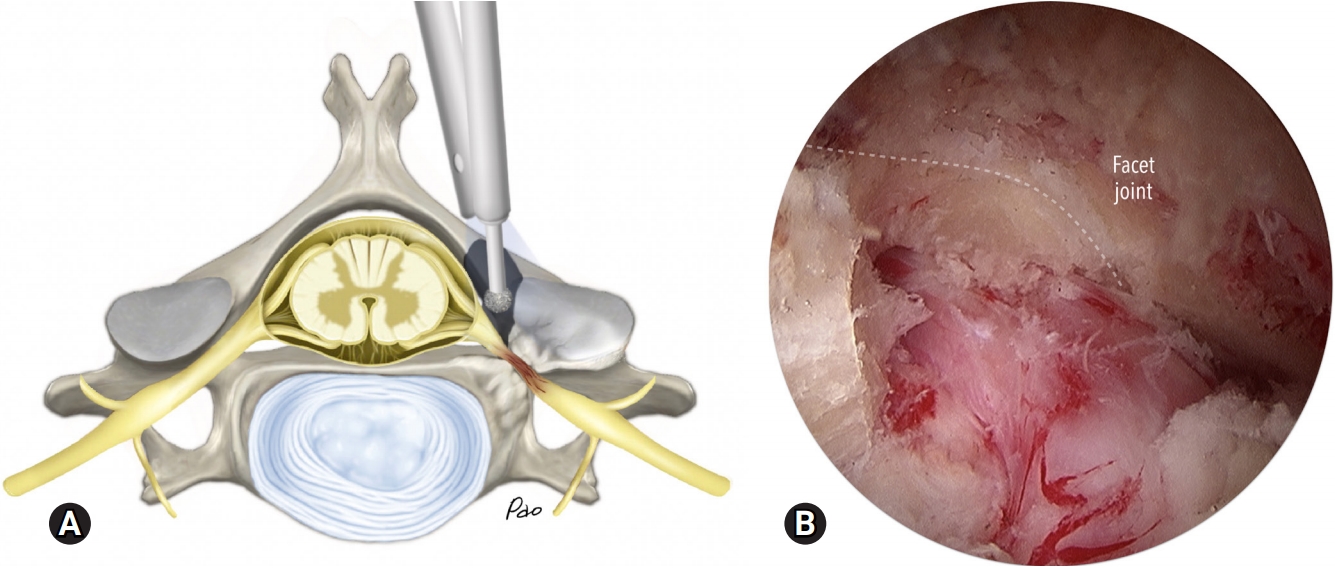
Fig. 5.An illustration (A) and an endoscopic photo (B) demonstrate the use of a curved osteotome to undercut the facet joint and decompress the nerve root. 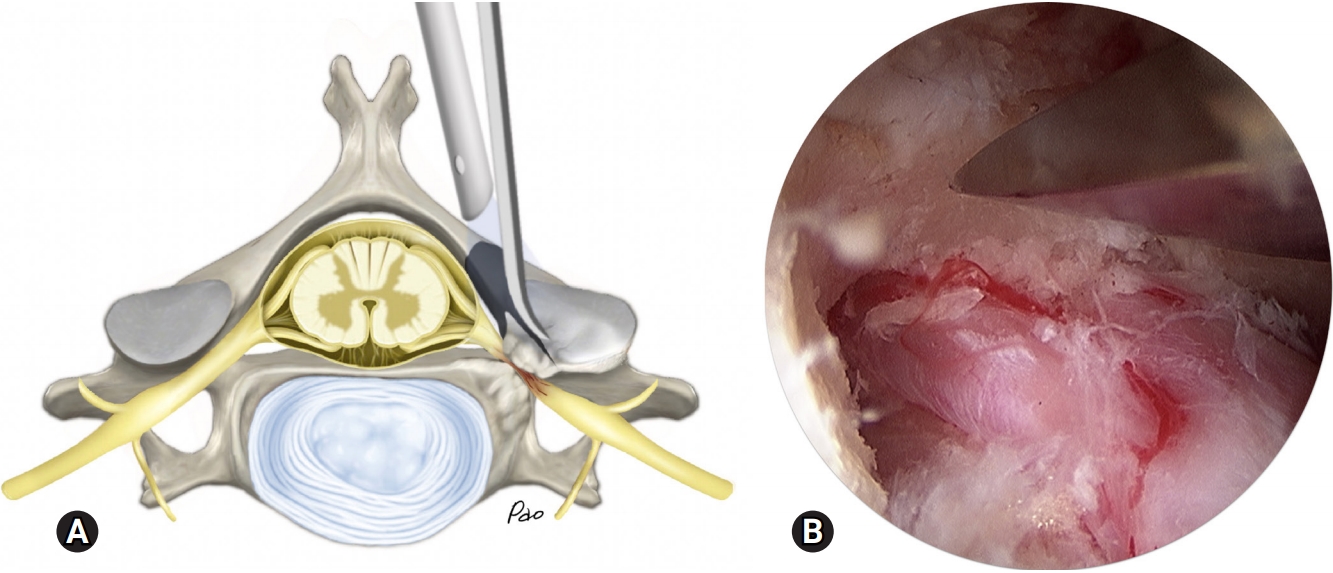
Fig. 6.An illustration (A) and an endoscopic photo (B) demonstrate complete decompression of the nerve root between the cranial and caudal pedicles. 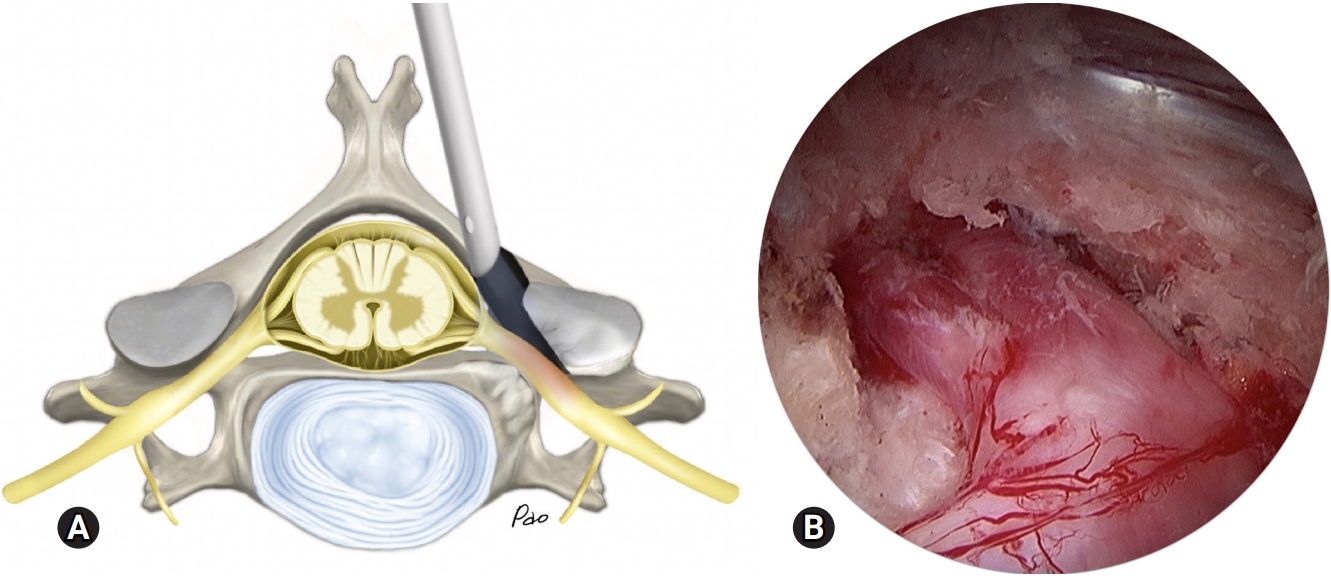
Fig. 7.A series of endoscopic photos shows a 62-year-old woman with left-side C5–6 foraminal stenosis. (A) The initial V-point (white asterisk). (B) Foraminotomy. (C) Elevation of the ligamentum flavum. (D) Removal of the perineural membrane. (E) Complete decompression of the nerve root viewed from inside of the foramen. (F) The extent of foraminotomy viewed posteriorly. Most of the ligamentum flavum is preserved. (G) A preoperative oblique sagittal magnetic resonance image shows the foraminal stenosis (white arrowhead). (H) A postoperative axial magnetic resonance image shows widening of the foramen with minimal destruction of the facet joint (white arrowheads). 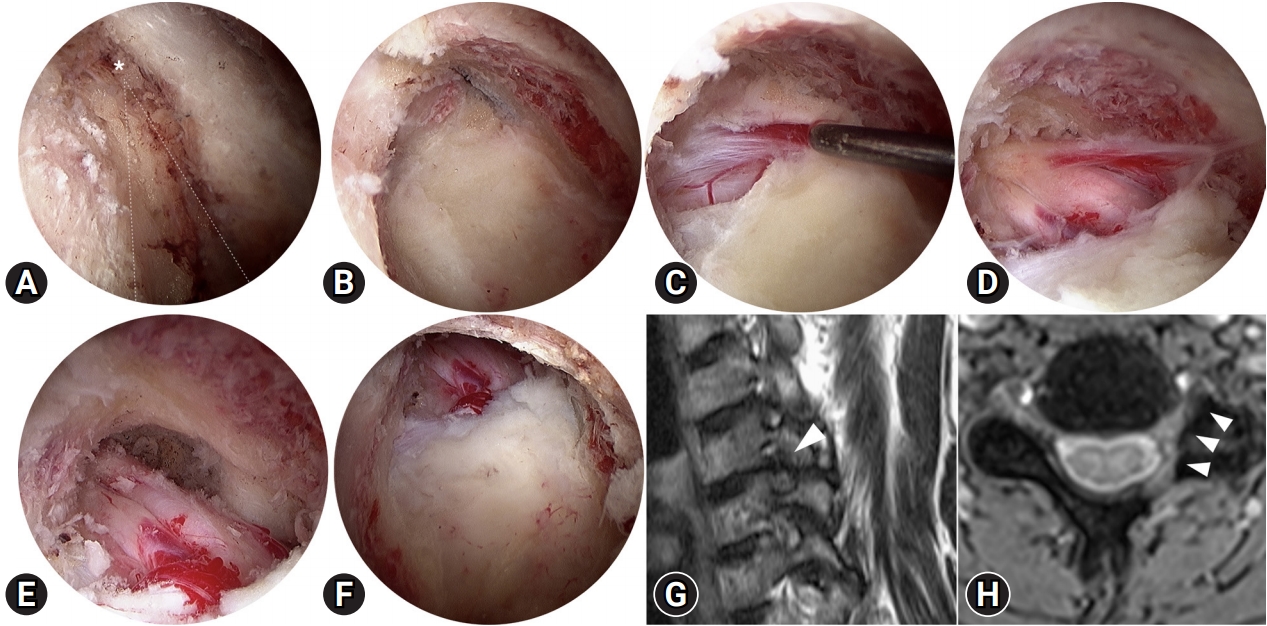
Fig. 8.Preoperative magnetic resonance images (A, B) reveal left-side foraminal stenosis (white arrowhead), caused by osteophytes originating from the uncovertebral joint in a 57-year-old male patient. (C, D) Postoperative magnetic resonance images demonstrate good decompression of the neural foramen (indicated by the white dashed circle). (E) A clinical photograph displays the cosmetic surgical wounds. 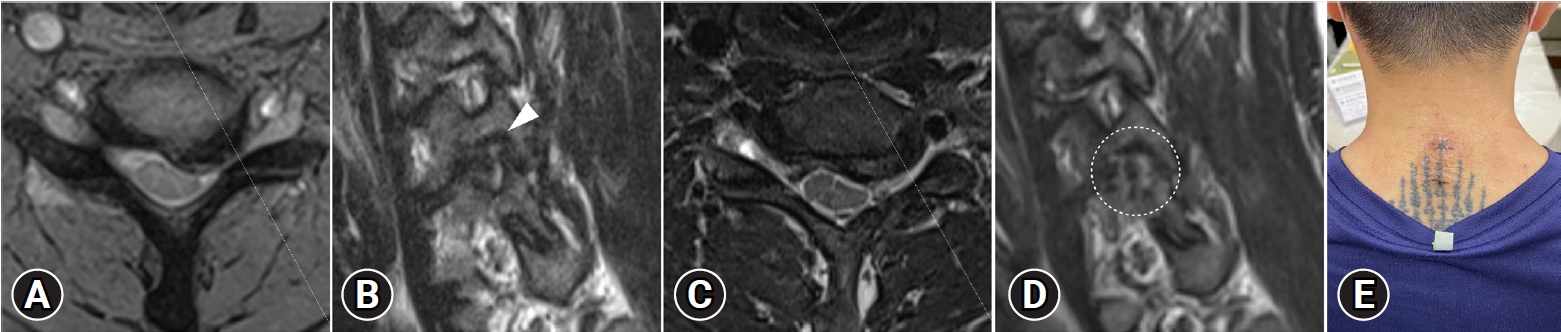
Fig. 9.(A) An axial magnetic resonance image taken before the operation shows stenosis in the left foramen. (B) An axial magnetic resonance image taken after the operation shows good decompression of the foramen (white asterisk) with 67.7% facet preservation. 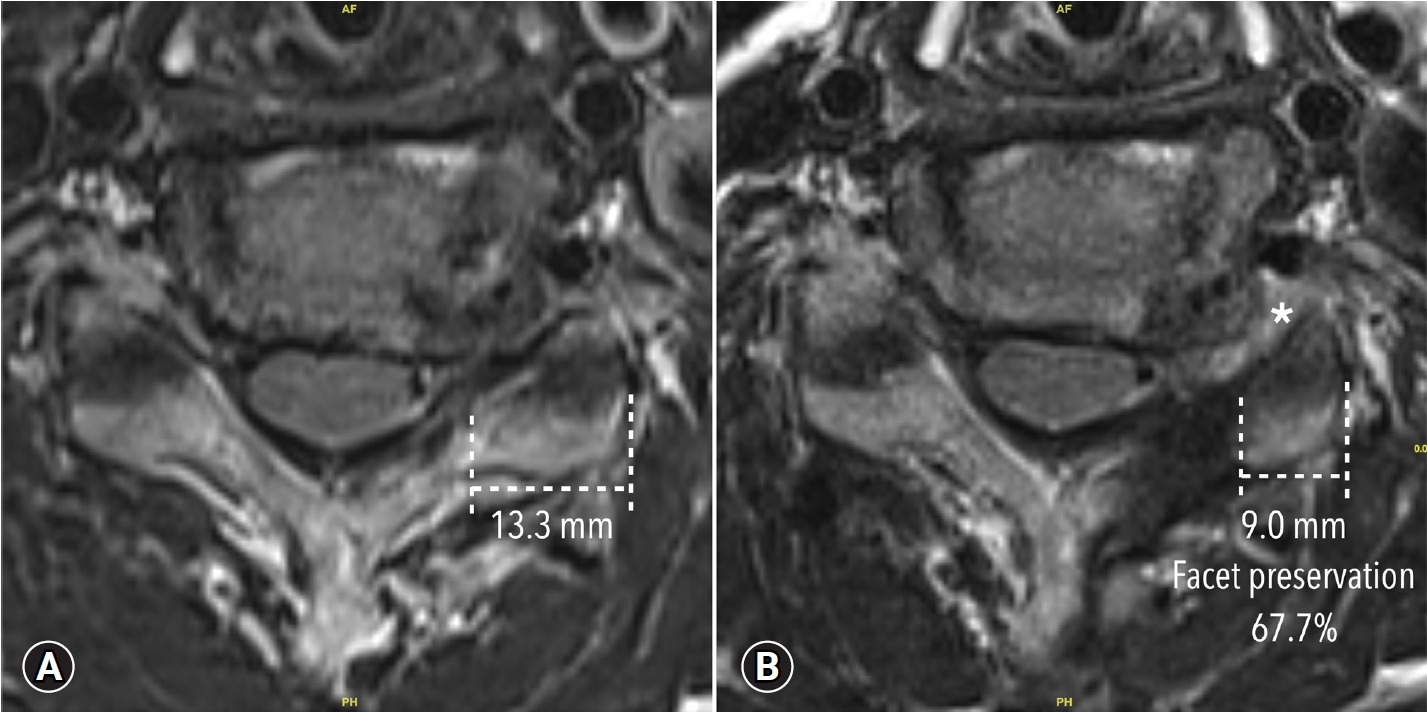
Fig. 10.Comparison of the contralateral inside-out (A) and ipsilateral (B) foraminotomy in terms of the extent of facet joint destruction (shaded areas), the viewing angles under the endoscope, and the ergonomics of using the surgical instruments. 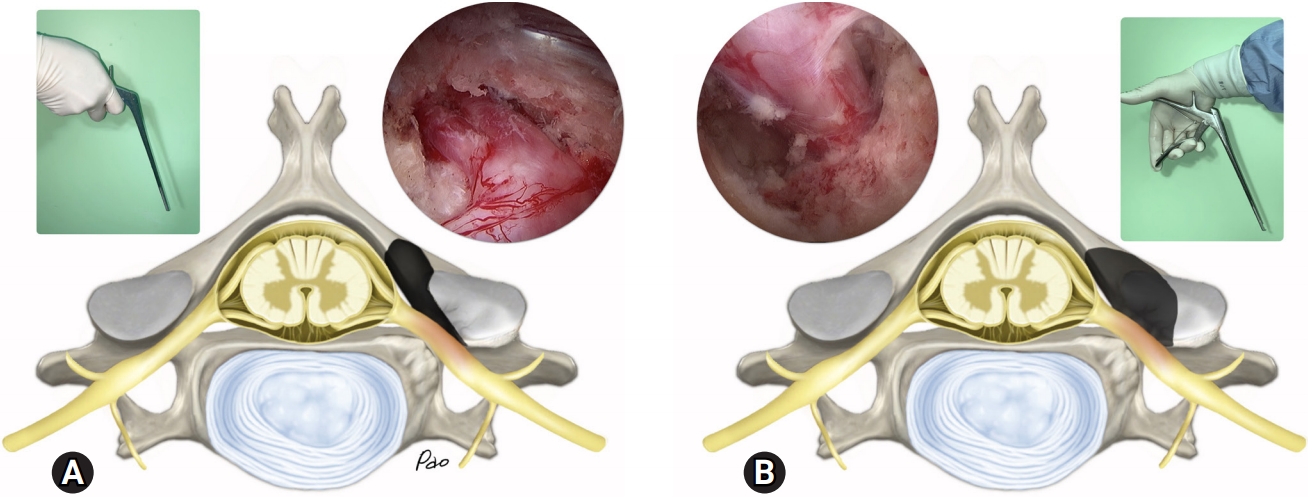
Table 1.Demographic data and clinical characteristics REFERENCES1. Zeng ZL, Zhu R, Wu YC, Zuo W, Yu Y, Wang JJ, et al. Effect of graded facetectomy on lumbar biomechanics. J Healthc Eng 2017;2017:7981513.
2. Abbed KM, Coumans JV. Cervical radiculopathy: pathophysiology, presentation, and clinical evaluation. Neurosurgery 2007;60:S28–S34.
3. Woods BI, Hilibrand AS. Cervical radiculopathy: epidemiology, etiology, diagnosis, and treatment. J Spinal Disord Tech 2015;28:E251–E259.
5. Fang W, Huang L, Feng F, Yang B, He L, Du G, et al. Anterior cervical discectomy and fusion versus posterior cervical foraminotomy for the treatment of single-level unilateral cervical radiculopathy: a meta-analysis. J Orthop Surg Res 2020;15:202.
6. Carrier CS, Bono CM, Lebl DR. Evidence-based analysis of adjacent segment degeneration and disease after ACDF: a systematic review. Spine J 2013;13:1370–1378.
7. Shriver MF, Lewis DJ, Kshettry VR, Rosenbaum BP, Benzel EC, Mroz TE. Pseudoarthrosis rates in anterior cervical discectomy and fusion: a meta-analysis. Spine J 2015;15:2016–2027.
8. Yee TJ, Swong K, Park P. Complications of anterior cervical spine surgery: a systematic review of the literature. J Spine Surg 2020;6:302–322.
9. Riew KD, Cheng I, Pimenta L, Taylor B. Posterior cervical spine surgery for radiculopathy. Neurosurgery 2007;60:S57–S63.
10. Dohrmann GJ, Hsieh JC. Long-term results of anterior versus posterior operations for herniated cervical discs: analysis of 6,000 patients. Med Princ Pract 2014;23:70–73.
11. Liu WJ, Hu L, Chou PH, Wang JW, Kan WS. Comparison of anterior cervical discectomy and fusion versus posterior cervical foraminotomy in the treatment of cervical radiculopathy: a systematic review. Orthop Surg 2016;8:425–431.
12. Ruetten S, Komp M, Merk H, Godolias G. Full-endoscopic cervical posterior foraminotomy for the operation of lateral disc herniations using 5.9-mm endoscopes: a prospective, randomized, controlled study. Spine (Phila Pa 1976) 2008;33:940–948.
13. Adamson TE. The impact of minimally invasive cervical spine surgery. Invited submission from the Joint Section Meeting on Disorders of the Spine and Peripheral Nerves, March 2004. J Neurosurg Spine 2004;1:43–46.
14. Deutsch H, Haid RW, Rodts GE, Mummaneni PV. Postlaminectomy cervical deformity. Neurosurg Focus 2003;15:E5.
16. Pao JL, Lin SM, Chen WC, Chang CH. Unilateral biportal endoscopic decompression for degenerative lumbar canal stenosis. J Spine Surg 2020;6:438–446.
17. Choi DJ, Kim JE. Efficacy of biportal endoscopic spine surgery for lumbar spinal stenosis. Clin Orthop Surg 2019;11:82–88.
18. Choi DJ, Kim JE, Jung JT, Kim YS, Jang HJ, Yoo B, et al. Biportal endoscopic spine surgery for various foraminal lesions at the lumbosacral lesion. Asian Spine J 2018;12:569–573.
19. Eun SS, Eum JH, Lee SH, Sabal LA. Biportal endoscopic lumbar decompression for lumbar disk herniation and spinal canal stenosis: a technical note. J Neurol Surg A Cent Eur Neurosurg 2017;78:390–396.
20. Kang MS, You KH, Choi JY, Heo DH, Chung HJ, Park HJ. Minimally invasive transforaminal lumbar interbody fusion using the biportal endoscopic techniques versus microscopic tubular technique. Spine J 2021;21:2066–2077.
21. Heo DH, Hong YH, Lee DC, Chung HJ, Park CK. Technique of biportal endoscopic transforaminal lumbar interbody fusion. Neurospine 2020;17:S129–S137.
22. Vernon H. The neck disability index: state-of-the-art, 1991-2008. J Manipulative Physiol Ther 2008;31:491–502.
23. Macnab I. Negative disc exploration. An analysis of the causes of nerve-root involvement in sixty-eight patients. J Bone Joint Surg Am 1971;53:891–903.
24. Matsumura A, Namikawa T, Terai H, Tsujio T, Suzuki A, Dozono S, et al. The influence of approach side on facet preservation in microscopic bilateral decompression via a unilateral approach for degenerative lumbar scoliosis. Clinical article. J Neurosurg Spine 2010;13:758–765.
25. Dohzono S, Matsumura A, Terai H, Toyoda H, Suzuki A, Nakamura H. Radiographic evaluation of postoperative bone regrowth after microscopic bilateral decompression via a unilateral approach for degenerative lumbar spondylolisthesis. J Neurosurg Spine 2013;18:472–478.
26. Henderson CM, Hennessy RG, Shuey HM Jr, Shackelford EG. Posterior-lateral foraminotomy as an exclusive operative technique for cervical radiculopathy: a review of 846 consecutively operated cases. Neurosurgery 1983;13:504–512.
27. Luyao H, Xiaoxiao Y, Tianxiao F, Yuandong L, Wang P. Management of cervical spondylotic radiculopathy: a systematic review. Global Spine J 2022;12:1912–1924.
28. Sahai N, Changoor S, Dunn CJ, Sinha K, Hwang KS, Faloon M, et al. Minimally invasive posterior cervical foraminotomy as an alternative to anterior cervical discectomy and fusion for unilateral cervical radiculopathy: a systematic review and meta-analysis. Spine (Phila Pa 1976) 2019;44:1731–1739.
29. Engquist M, Löfgren H, Öberg B, Holtz A, Peolsson A, Söderlund A, et al. A 5- to 8-year randomized study on the treatment of cervical radiculopathy: anterior cervical decompression and fusion plus physiotherapy versus physiotherapy alone. J Neurosurg Spine 2017;26:19–27.
30. Jagannathan J, Sherman JH, Szabo T, Shaffrey CI, Jane JA. The posterior cervical foraminotomy in the treatment of cervical disc/osteophyte disease: a single-surgeon experience with a minimum of 5 years’ clinical and radiographic follow-up. J Neurosurg Spine 2009;10:347–356.
31. Chung SW, Kim HJ, Lee SH, Lee SY, Kang MS, Shin YH, et al. Posterior cervical foraminotomy for cervical radiculopathy: should cervical alignment be considered? J Spine Surg 2019;5:541–548.
32. Foley KT, Smith MM. Microendoscopic discectomy. Tech Neurosurg 1997;3:301–307.
33. Roh SW, Kim DH, Cardoso AC, Fessler RG. Endoscopic foraminotomy using MED system in cadaveric specimens. Spine (Phila Pa 1976) 2000;25:260–264.
34. Burke TG, Caputy A. Microendoscopic posterior cervical foraminotomy: a cadaveric model and clinical application for cervical radiculopathy. J Neurosurg 2000;93:126–129.
35. Hilton DL Jr. Minimally invasive tubular access for posterior cervical foraminotomy with three-dimensional microscopic visualization and localization with anterior/posterior imaging. Spine J 2007;7:154–158.
36. Coric D, Adamson T. Minimally invasive cervical microendoscopic laminoforaminotomy. Neurosurg Focus 2008;25:E2.
37. Nomura K, Yoshida M. Assessment of the learning curve for microendoscopic decompression surgery for lumbar spinal canal stenosis through an analysis of 480 cases involving a single surgeon. Global Spine J 2017;7:54–58.
38. Song KS, Lee CW. The biportal endoscopic posterior cervical inclinatory foraminotomy for cervical radiculopathy: technical report and preliminary results. Neurospine 2020;17:S145–S153.
39. Choi CM. Biportal endoscopic spine surgery (BESS): considering merits and pitfalls. J Spine Surg 2020;6:457–465.
40. Jang JW, Lee DG, Park CK. Rationale and advantages of endoscopic spine surgery. Int J Spine Surg 2021;15:S11–S20.
41. Heo DH, Lee DC, Park CK. Comparative analysis of three types of minimally invasive decompressive surgery for lumbar central stenosis: biportal endoscopy, uniportal endoscopy, and microsurgery. Neurosurg Focus 2019;46:E9.
42. Pranata R, Lim MA, Vania R, July J. Biportal endoscopic spinal surgery versus microscopic decompression for lumbar spinal stenosis: a systematic review and meta-analysis. World Neurosurg 2020;138:e450–e458.
43. Ito Z, Shibayama M, Nakamura S, Yamada M, Kawai M, Takeuchi M, et al. Clinical comparison of unilateral biportal endoscopic laminectomy versus microendoscopic laminectomy for single-level laminectomy: a single-center, retrospective analysis. World Neurosurg 2021;148:e581–e588.
44. Iwai H, Inanami H, Koga H. Comparative study between full-endoscopic laminectomy and microendoscopic laminectomy for the treatment of lumbar spinal canal stenosis. J Spine Surg 2020;6:E3–E11.
|
|
|||||||||||||||||||||||||||||||||||||||||